Can an Eye Doctor Help With Dry Eyes?
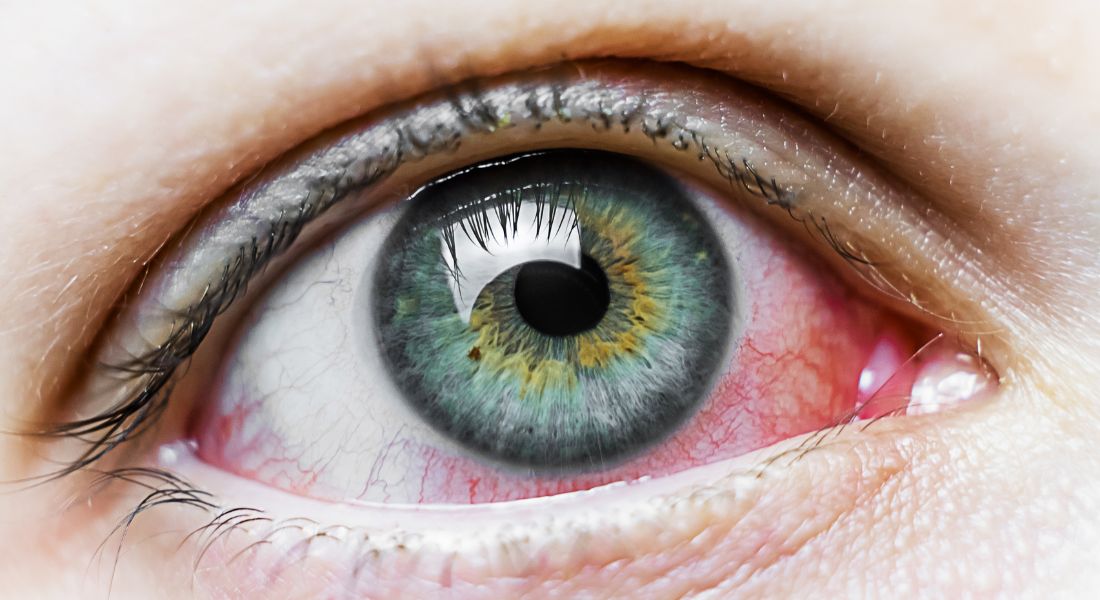
Dry eyes can sound like a small problem until you are the one dealing with them every day. When your eyes feel gritty, sore, watery, tired, or irritated, it can affect almost everything you do. You may notice discomfort when reading, working on a screen, driving, watching television, wearing contact lenses, or going outside in windy weather. Even simple daily tasks can start to feel frustrating when your eyes never feel fully comfortable.
So, can an eye doctor help with dry eyes? Yes, absolutely. An eye doctor can help diagnose the cause of your dry eye symptoms, assess the health of your tear film, check for related eyelid or surface problems, and recommend a treatment plan that suits your specific condition.
This matters because dry eye is not always just “not enough tears.” It can happen when your eyes do not produce enough tears, when your tears evaporate too quickly, or when the quality of your tears is poor. Moorfields explains that dry eye is a condition where there is a problem with tear production, while the American Academy of Ophthalmology describes dry eye as occurring when the eyes do not make enough tears or the tears do not work properly.
That means two people can both say, “My eyes feel dry,” but need different treatments. One person may need lubricating drops. Another may need eyelid treatment. Another may have inflammation, meibomian gland dysfunction, allergy, contact lens-related irritation, medication-related dryness, or an underlying health condition. This is why seeing an eye doctor can be so useful. Instead of guessing which eye drops to buy, you can find out what is actually causing your symptoms and what will help your eyes feel more comfortable.
What Does Dry Eye Feel Like?
Dry eye can feel different from person to person. You may feel burning, stinging, scratchiness, grittiness, or a foreign body sensation, as if something is stuck in your eye. You may also notice redness, watering, blurred vision, heaviness, light sensitivity, or general eye fatigue.
Some people describe it as a sandy feeling. Others say their eyes feel tired all the time, even after sleep. You may also feel that your vision clears when you blink, then becomes blurry again after a few seconds. Dry eye can also make your eyes water. This often surprises people because watery eyes do not sound “dry.”
However, when the eye surface becomes irritated, your eyes may produce reflex tears, which are often watery and unstable rather than properly lubricating. So, if your eyes are constantly watering, dry eye can still be part of the problem. You may also notice that symptoms are worse at certain times of day. For example, your eyes may feel more uncomfortable in the evening after screen work, or first thing in the morning if your eyelids and tear film are affected overnight. These patterns help your eye doctor understand what is happening.
Why Dry Eye Should Not Be Ignored
Mild dry eye may come and go. You may feel it after a long day on your laptop, after travelling, or after spending time in air conditioning. If symptoms settle quickly, you may not think much about it. But ongoing dry eye should not be ignored.
When the eye surface remains dry or irritated, it can affect comfort, vision, contact lens tolerance, sleep quality, work productivity, and quality of life. Your eyes need a healthy tear film to stay clear and comfortable. The tear film protects the surface of the eye, keeps vision smooth, washes away tiny particles, and helps reduce irritation. When that tear film is unstable, your eyes can feel constantly uncomfortable.
Over time, untreated dry eye may also lead to inflammation of the eye surface. This can create a cycle where dryness causes irritation, irritation causes inflammation, and inflammation makes dryness worse. An eye doctor can help break this cycle. Instead of only treating symptoms for a few minutes at a time, the aim is to understand the cause and manage the condition properly.
Why Your Eyes Need Tears
Tears are not just water. They are made up of different layers that work together to keep your eyes moist, smooth, and protected. A healthy tear film usually includes an oily layer, a watery layer, and a mucus layer. Each layer has a job. The oily layer helps slow evaporation.
The watery layer provides moisture. The mucus layer helps tears spread evenly across the eye surface. If one part of this system is not working well, dry eye symptoms can appear. For example, if the oily layer is poor, your tears may evaporate too quickly. If the watery layer is reduced, your eyes may not have enough moisture.
If the tear film does not spread properly, vision may fluctuate and the eyes may feel irritated. This is one reason over-the-counter drops do not always solve the problem. They may temporarily replace moisture, but they may not correct the reason your tears are unstable. An eye doctor can look at how your tear film is functioning and whether your eyelids, glands, inflammation, or environment are contributing.
Common Causes of Dry Eyes
Dry eyes can have many causes. Age is one common factor because tear production and tear quality can change over time. Many people notice symptoms more often as they get older. Screen use is another major trigger. When you look at a screen, you tend to blink less often. Your blink may also become incomplete, which means the tear film is not spread properly across the eye surface. Environment can also make symptoms worse.
Air conditioning, heating, wind, smoke, dry air, fans, and low humidity can all increase tear evaporation. You may notice this more in offices, cars, aeroplanes, or heated rooms. Contact lenses can also contribute. They sit on the eye surface and can interfere with the tear film, especially if you wear them for long hours or already have mild dryness. Some medications can make dry eye worse too.
These may include certain antihistamines, antidepressants, blood pressure medicines, acne medicines, and hormone-related treatments. You should never stop medication without medical advice, but it is worth mentioning your medicines during an eye appointment. Medical conditions may also be involved. Autoimmune conditions, thyroid disease, diabetes, rosacea, blepharitis, and eyelid problems can all be linked with dry eye symptoms. Because there are so many possible causes, proper diagnosis matters.
How an Eye Doctor Diagnoses Dry Eye
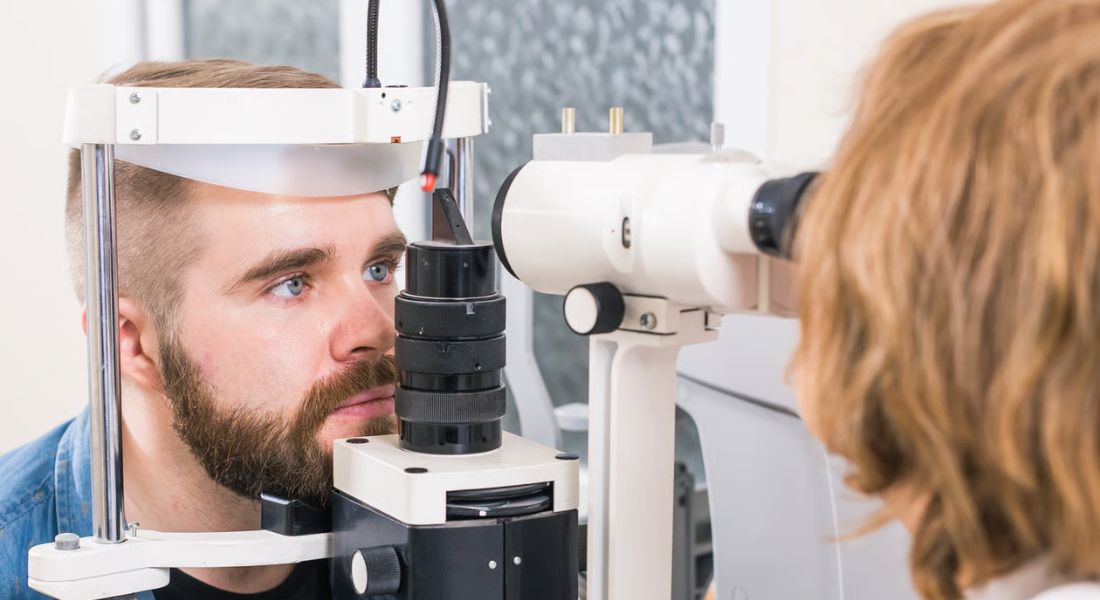
Diagnosis usually starts with a detailed discussion about your symptoms. Your eye doctor may ask when the dryness began, whether one or both eyes are affected, and what makes the discomfort better or worse. They may also ask about redness, watering, blurred vision, pain, itching, or light sensitivity. This helps them understand whether your symptoms are mild, ongoing, or linked to a specific trigger.
- Reviewing Your Symptoms and Lifestyle: Your eye doctor will usually ask about your daily habits, including screen time, contact lens use, and your work environment. They may also ask about medication, medical history, previous eye surgery, or any health conditions that could affect tear production.
- Examining the Eye Surface: The eye doctor may carefully examine your eyelids, tear film, cornea, conjunctiva, lashes, and meibomian glands. This helps them check whether your eyes are producing enough tears and whether the tear film is protecting the eye surface properly.
- Using a Slit Lamp and Special Dyes: A slit lamp may be used to examine the eye in detail under magnification. Special dyes can also be applied to reveal dry patches, surface damage, or areas where the tear film is breaking down too quickly.
- Checking Tear Stability and Tear Production: Your tear break-up time may be assessed to see how quickly your tear film becomes unstable after blinking. In some cases, tear production may also be measured, especially if your symptoms suggest that your eyes are not making enough tears.
The exact tests used can vary depending on your symptoms and the equipment available at the clinic. However, the aim is always to understand the type, cause, and severity of your dry eye. This is important because dry eye is not the same for everyone, and treatment works best when it is matched to the underlying problem. A proper diagnosis can help your eye doctor create a more suitable treatment plan for long-term comfort.
Why Diagnosis Is Better Than Guessing
It is common to buy eye drops from a pharmacy when your eyes feel dry. That can be a reasonable first step for mild symptoms. However, if dryness keeps returning, it is better to get your eyes checked. The problem with guessing is that dry eye has different types. If your tears evaporate too quickly because of meibomian gland dysfunction, you may need eyelid-focused treatment.
If inflammation is involved, lubricants alone may not be enough. If allergies are causing irritation, the treatment may be different again. You may also be using drops that are not ideal for your eyes. Some drops contain preservatives, which can irritate sensitive eyes if used frequently. Moorfields Private advises preservative-free drops in severe symptoms, frequent drop use, or contact lens wear.
That does not mean all preserved drops are bad. It means the right choice depends on your symptoms, frequency of use, eye surface health, and whether you wear contact lenses. An eye doctor can guide you instead of leaving you to trial one product after another.
Can Dry Eye Cause Blurry Vision?
Yes, dry eye can cause blurry or fluctuating vision. Your tear film is the first smooth surface that light passes through before entering the eye. If that surface is unstable, your vision may become temporarily blurred. You may notice that blinking clears the blur for a moment. Then the blur returns as the tear film breaks up again.
This can be especially noticeable when reading, driving, working on a screen, or focusing for long periods. Dry eye-related blur can be frustrating because it may come and go. You may feel that your glasses are not working properly, even when the prescription is correct. However, blurred vision should always be taken seriously.
If your vision changes suddenly, becomes significantly reduced, or is accompanied by pain, redness, flashes, floaters, halos, or severe headache, you should seek urgent medical advice. If the blur is mild, fluctuating, and linked to dryness, an eye exam can still help confirm the cause and guide treatment.
Can Dry Eye Cause Eye Pain?
Dry eye can cause discomfort, soreness, burning, and aching. In some cases, it can feel painful, especially if the eye surface is very irritated. However, severe eye pain is not something you should dismiss as dryness. Pain with redness, light sensitivity, reduced vision, discharge, injury, or contact lens wear should be checked promptly.
Dry eye discomfort often feels like burning, grittiness, scratchiness, or tiredness. It may worsen through the day, in dry environments, or after screen use. If your pain is sharp, intense, one-sided, or unusual for you, it is better to seek professional advice quickly. An eye doctor can check whether the pain is due to dry eye or another eye condition that needs different treatment.
Treatment Option 1: Artificial Tears
Artificial tears are often the first treatment for mild to moderate dry eye. These are lubricating eye drops designed to support the tear film and reduce dryness. They can help relieve burning, grittiness, and fluctuating vision. There are many types of artificial tears.
Some are thinner and feel light. Others are thicker and last longer but may blur vision briefly after use. You may need to try a suitable formulation based on your symptoms. If you use drops often, preservative-free options may be recommended. This is especially relevant if your eyes are sensitive, symptoms are severe, or you wear contact lenses.
The American Academy of Ophthalmology notes that artificial tears are commonly used to add tears as part of dry eye treatment. Artificial tears can help, but they are not always the full answer. If inflammation, eyelid disease, or gland dysfunction is present, additional treatment may be needed.
Treatment Option 2: Gels and Ointments
Eye gels and ointments can be helpful when symptoms are stronger or when dryness is worse overnight. They stay on the eye surface longer than standard drops. The downside is that they can blur your vision temporarily. This is why ointments are often used at bedtime rather than during the day.
If you wake with dry, sore, or sticky-feeling eyes, night-time lubrication may help. However, morning symptoms can also be linked to eyelid problems, incomplete eyelid closure, or inflammation. An eye doctor can advise whether gels or ointments are suitable for you. They can also help you avoid using products that may not match your specific dry eye type.
Treatment Option 3: Warm Compresses
Warm compresses are often recommended when meibomian gland dysfunction is involved. The aim is to gently warm the oil glands in the eyelids so the oil can flow more easily into the tear film. This may help reduce tear evaporation.
However, the technique matters. A quick splash of warm water is usually not enough. You may need consistent heat for several minutes, using a suitable heated eye mask or compress. Your eye doctor can show you how to do this safely.
They may also advise eyelid massage or cleaning, depending on your eyelid condition. Warm compresses can be useful, but they are not suitable for every eye problem. If your eyes are very red, painful, infected, or inflamed, you should seek advice before starting home treatment.
Treatment Option 4: Eyelid Hygiene
Eyelid hygiene can be helpful when blepharitis or lid margin disease is contributing to dry eye symptoms. These conditions can cause inflammation around the eyelids, especially near the base of the lashes. When this area becomes irritated, it can affect the tear film and make your eyes feel dry, gritty, or uncomfortable.
This care usually involves gently cleaning the eyelid margins with recommended wipes, solutions, or safe techniques. The aim is to reduce debris, oil build-up, crusting, and irritation around the lashes. Although it may seem like a small step, it can make a noticeable difference when eyelid inflammation is part of the problem.
You should avoid harsh soaps, strong cleansers, or random home remedies around the eyes because the eyelid skin and eye surface are delicate. Irritating products may make dryness, redness, or stinging worse. An eye doctor can recommend a safe routine, and consistency is important because eyelid-related dry eye often needs ongoing management.
Treatment Option 5: Anti-Inflammatory Treatment
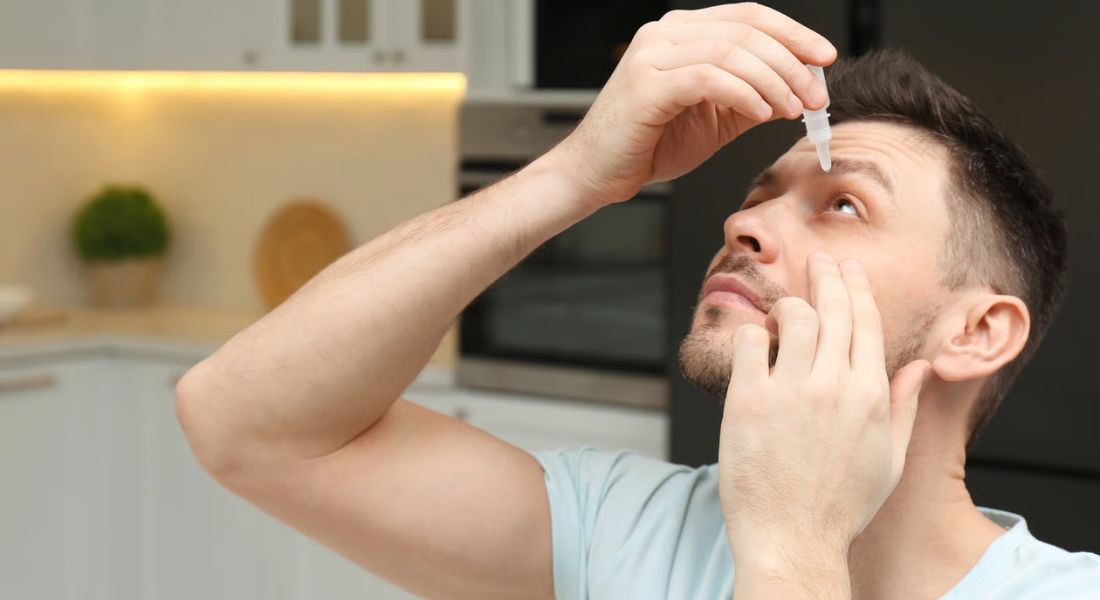
Dry eye can sometimes involve inflammation, which means lubricating drops may not be enough on their own. When the eye surface is inflamed, symptoms such as burning, redness, irritation, and discomfort may continue even if you use artificial tears. In these cases, an eye doctor may recommend anti-inflammatory eye drops or other suitable treatments based on your condition.
These treatments are usually chosen carefully because not every medicine is suitable for every patient. Steroid drops may be used in some cases for short-term control, especially when inflammation needs to be reduced quickly. Other prescription treatments may be considered for longer-term management, depending on your diagnosis, availability, and clinical judgement.
The American Academy of Ophthalmology’s dry eye treatment guidance includes options such as artificial tears, punctal plugs, steroid or other medicines, and avoiding dry or windy environments. You should not use prescription eye medication without professional guidance, as the wrong treatment may be ineffective or harmful. An eye doctor can assess your eyes properly and recommend the safest option for your needs.
Treatment Option 6: Punctal Plugs
Punctal plugs may be considered for some people with dry eye, especially when tear volume is low. These are tiny devices placed in the tear drainage openings to help keep tears on the eye surface for longer. They do not make your eyes produce more tears, but they can reduce how quickly your existing tears drain away.
This option may be helpful in selected cases, but it is not suitable for everyone. If inflammation is significant, your eye doctor may want to treat that first before considering plugs. Keeping poor-quality or inflammatory tears on the eye surface may not always be ideal, as this could continue to irritate the eyes.
That is why punctal plugs should be used carefully and only when they are appropriate for your condition. An eye doctor can assess your tear production, symptoms, and eye surface health before deciding whether this treatment is suitable. This helps make sure the treatment supports your eye comfort rather than making the underlying problem worse.
Treatment Option 7: Treating Meibomian Gland Dysfunction
If your dry eye is mainly evaporative, meibomian gland dysfunction may be an important area to treat. This happens when the oil-producing glands in the eyelids do not work as well as they should. As a result, the tear film may become unstable, and your tears may evaporate too quickly.
Treatment may include warm compresses, eyelid hygiene, gland expression, in-clinic therapies, or medication in selected cases. The aim is to improve the oily layer of the tear film so your tears stay on the eye surface for longer. When this oily layer improves, your eyes may feel less dry, irritated, or uncomfortable.
This type of dry eye often needs ongoing care rather than a one-time treatment. Your symptoms may improve with treatment, but they can return if eyelid maintenance stops completely. An eye doctor can help you build a realistic routine that you can actually follow, instead of one that feels too difficult after a week.
Treatment Option 8: Managing Allergies
Allergy and dry eye can overlap, which means the symptoms may feel very similar. Both can cause irritation, watering, redness, and general discomfort in the eyes. However, itching is often more noticeable with allergy, so this symptom can be an important clue.
If you have allergy-related symptoms, standard dry eye treatment may not fully solve the problem on its own. You may also need allergy management, such as avoiding triggers, using suitable anti-allergy drops, or treating eyelid inflammation. The right approach depends on what is actually causing your symptoms.
It is important not to self-treat red, itchy, or irritated eyes for months without a proper diagnosis. Some people use the wrong drops for too long and end up making the irritation worse. An eye doctor can check whether your symptoms are mainly due to dry eye, allergy, blepharitis, or a combination of these issues.
Treatment Option 9: Reviewing Your Environment
Your surroundings can make dry eye symptoms worse, even if they are not the main cause. Air conditioning, heating, fans, smoke, dust, pollution, wind, and low humidity can all increase irritation. These factors can make your tears evaporate more quickly and leave your eyes feeling dry, gritty, or uncomfortable.
You may not be able to control every environment, but small changes can still help. Try avoiding direct airflow towards your face, adjust car vents away from your eyes, and consider using a humidifier if indoor air is very dry. Wearing sunglasses outdoors on windy days can also help protect your eyes from wind, dust, and irritation.
Screen habits also matter because you may blink less when you are concentrating. Taking regular breaks from screens and making an effort to blink fully can reduce the daily burden on your eyes. Your eye doctor may ask about your work and home environment because dry eye treatment is not only about drops; lifestyle and surroundings matter too.
Treatment Option 10: Reviewing Medication and Health Conditions
Some medicines can contribute to dry eye symptoms, so your eye doctor may ask about your medication list. This can provide useful clues about why your eyes feel dry, irritated, or uncomfortable. You should not stop any prescribed medicine without speaking to the doctor who manages it, but your GP or specialist may be able to review options if a medicine is contributing to dryness.
Health conditions can also play an important role in dry eye. Autoimmune disease, thyroid problems, rosacea, diabetes, and hormonal changes may all affect the eyes and tear film. When dry eye is linked to a wider health issue, treating the eyes alone may not always be enough.
If your dry eye is severe, persistent, or linked with symptoms such as dry mouth, joint pain, skin changes, or other concerns, further medical evaluation may be needed. Your eyes can sometimes reflect what is happening elsewhere in the body. This is another reason why a proper assessment matters before choosing the right treatment plan.
What If Over-the-Counter Drops Are Not Working?
If you have tried over-the-counter drops and your eyes still feel uncomfortable, it may be time to book an eye appointment. There are several reasons why drops may not be helping enough. You may be using them too infrequently, you may need a different formulation, or you may need preservative-free drops.
Your dryness may also be caused by something that simple lubricating drops cannot fully manage. For example, you may have eyelid gland dysfunction, inflammation, allergy, or another eye surface problem. In some cases, you may be treating the symptom rather than the actual cause.
If your tears evaporate too quickly because the oil glands are blocked, watery drops may only give short-term relief. This does not mean you are doing anything wrong; it simply means dry eye can be more complex than it first appears. An eye doctor can assess the cause properly and help you move beyond trial and error.
When Should You See an Eye Doctor for Dry Eyes?
You should see an eye doctor if your dry eye symptoms are frequent, persistent, worsening, or affecting your daily life. You should also book an appointment if your eyes feel red, sore, gritty, watery, light-sensitive, or blurry. If your symptoms keep returning despite using drops, it may mean there is an underlying cause that needs proper assessment.
If you wear contact lenses and dryness is making them uncomfortable, you should also get checked. You should seek advice if you need drops many times a day, as this may suggest your dry eye needs a more suitable treatment plan. Moorfields Private notes that people with severe symptoms, frequent drop use of more than six times daily, or contact lens wear may be advised to use preservative-free drops.
You should seek urgent advice if you have severe pain, sudden vision loss, significant light sensitivity, injury, chemical exposure, or a red painful eye with reduced vision. These symptoms may not be simple dry eye and should not be ignored. It is always safer to get checked so the right cause can be identified and treated properly.
What Happens During a Dry Eye Appointment?
Your dry eye appointment will usually begin with a detailed discussion about your symptoms. Your eye doctor will ask what your eyes feel like, how long the problem has been happening, and what seems to make it better or worse. They may also ask whether your eyes feel worse in the morning, later in the day, or after certain activities. These details help them understand the pattern of your dry eye symptoms.
- Discussing Your Symptoms: Your eye doctor may ask whether your eyes feel dry, gritty, burning, watery, itchy, or sensitive to light. They may also ask if your vision becomes blurry during the day or after activities such as reading, driving, or using screens.
- Reviewing Your Daily Habits and Triggers: You may be asked about screen use, contact lenses, makeup, skincare products, heating, air conditioning, allergies, medication, and your work environment. These factors can often contribute to dry eye or make existing symptoms worse.
- Examining Your Eyes Carefully: Your doctor may check your eyelids, lashes, oil glands, tear film, eye surface, cornea, conjunctiva, and vision. This examination helps identify whether the dryness is linked to tear quality, tear quantity, eyelid health, or irritation on the eye surface.
- Checking Tear Evaporation and Surface Dryness: A special dye may be used to highlight dry patches, irritation, or damage on the eye surface. Your doctor may also assess how quickly your tears evaporate after blinking, which can show whether your tear film is stable or breaking up too quickly.
Together, these checks help your eye doctor understand whether your dry eye is mild, moderate, or severe. They also help identify what may be causing the problem, rather than only treating the symptoms. This is important because dry eye can have different causes, including screen habits, contact lenses, oil gland problems, allergies, or environmental triggers. Once the cause is clearer, your doctor can recommend the most suitable treatment to improve comfort and protect your eye surface.
Can Dry Eye Be Cured?
Dry eye can often be managed very effectively, but it is not always cured permanently. Some cases are temporary, especially when dryness is linked to a short-term trigger such as dry weather, medication changes, screen strain, or temporary irritation. Once the cause is addressed, the symptoms may improve or settle completely.
Other cases of dry eye can be long-term and may need ongoing care. This is more likely when dry eye is linked to age, eyelid gland dysfunction, rosacea, autoimmune disease, hormonal changes, or chronic inflammation. This does not mean you have to live with constant discomfort, but it does mean treatment may focus on control, comfort, and reducing flare-ups.
Many people feel much better once they have the right plan in place. The key is consistency because dry eye often improves when you combine the right drops, eyelid care, environmental changes, and medical treatment where needed. An eye doctor can help you understand whether your dry eye is temporary or long-term and guide you towards the most suitable management plan.
Can Diet Help Dry Eyes?
Diet may play a supporting role in eye health, but it is not usually a complete treatment for dry eyes by itself. Some people ask about omega-3 supplements, hydration, or anti-inflammatory diets when looking for ways to improve symptoms. However, the evidence and recommendations can vary depending on the individual and the type of dry eye they have.
Staying hydrated is sensible for your general health, and a balanced diet may support overall wellbeing. However, you should not rely on supplements alone if your dry eye symptoms are persistent, worsening, or affecting your daily comfort. Dry eye often needs a more targeted approach, especially when eyelid glands, inflammation, allergies, or tear film problems are involved.
If you are considering supplements, it is best to ask a healthcare professional first, especially if you take medication or have a medical condition. Some supplements may not be suitable for everyone or may interact with other treatments. Your eye doctor can advise whether diet is relevant to your situation and whether it should form part of your wider dry eye management plan.
Why Personalised Treatment Matters

Dry eye treatment should be personalised because not everyone has the same cause or severity of symptoms. Your tear film, eyelid health, age, contact lens use, work habits, medical history, and environment can all affect your eyes. A generic approach may help for a short time, but it may not give lasting relief if the real cause is not addressed.
For example, someone with mild screen-related dryness may improve with lubricating drops and better screen habits. Someone with meibomian gland dysfunction may need eyelid treatment to improve the oily layer of the tear film. Someone with inflammatory dry eye may need prescription treatment, while someone with severe aqueous tear deficiency may need a more advanced plan.
This is why an eye doctor’s assessment is valuable. It helps identify what is causing your dry eye and how much it is affecting the eye surface. Once the cause is clearer, your treatment can be matched to your needs instead of relying on trial and error.
How Long Does Treatment Take to Work?
Some dry eye treatments can work quite quickly, while others need more time. Lubricating drops may give relief within minutes, but the effect can be temporary, especially if the underlying cause is still present. This means your eyes may feel better for a short while, but the dryness or irritation may return later in the day.
Other treatments usually take longer to show their full benefit. Eyelid hygiene, warm compresses, anti-inflammatory treatment, and gland-focused care may need several weeks of consistent use before you notice clear improvement. This can feel frustrating, but it is normal because dry eye often develops gradually and may not settle overnight.
Your eye doctor may review your progress and adjust your plan if needed. If a treatment is not helping, you should not simply give up or keep changing products on your own. It is better to ask whether the diagnosis needs refining or whether another treatment approach may suit your eyes better.
Living With Dry Eye Day to Day
Managing dry eye often involves small daily habits that support your eyes over time. You should use your drops as advised, take screen breaks before your eyes become painful, and try to blink fully during focused tasks. These simple steps can help reduce strain and keep your eyes more comfortable throughout the day.
Your surroundings and eyelid care can also make a difference. Avoid direct air from fans or vents, protect your eyes outdoors, and use warm compresses if they have been recommended. If your eye doctor has advised eyelid cleaning, keeping the eyelids clean can also help reduce irritation and support a healthier tear film.
These steps may seem basic, but dry eye often responds best to regular care rather than occasional treatment during flare-ups. Think of it as looking after the eye surface every day, not just when symptoms become difficult. The goal is to reduce irritation, support your tear film, and keep your vision comfortable.
FAQs:
- Can an eye doctor help with dry eyes?
Yes, an eye doctor can diagnose the cause of dry eyes, check your tear film, examine your eyelids and eye surface, and recommend a treatment plan based on your symptoms. - What are the common symptoms of dry eyes?
Common symptoms include burning, stinging, grittiness, redness, watering, blurry vision, eye fatigue, light sensitivity, and the feeling that something is stuck in your eye. - Why do my eyes water if they are dry?
Dry eyes can sometimes cause watery eyes because irritation triggers reflex tears. These tears may water your eyes, but they may not lubricate the eye surface properly. - What causes dry eyes?
Dry eyes can be caused by ageing, screen use, contact lenses, air conditioning, heating, wind, certain medications, eyelid problems, allergies, and medical conditions such as diabetes, thyroid disease, rosacea, or autoimmune conditions. - How does an eye doctor diagnose dry eye?
An eye doctor may ask about your symptoms, screen use, contact lenses, medication, and medical history. They may also examine your eyelids, tear film, cornea, conjunctiva, and meibomian glands using specialist equipment. - Can dry eyes cause blurry vision?
Yes, dry eyes can cause blurry or fluctuating vision because the tear film helps create a smooth surface for clear sight. You may notice that blinking clears your vision briefly before the blur returns. - What treatments can help dry eyes?
Treatment may include artificial tears, preservative-free drops, eye gels, ointments, warm compresses, eyelid hygiene, anti-inflammatory drops, punctal plugs, allergy management, or treatment for meibomian gland dysfunction. - When should I see an eye doctor for dry eyes?
You should see an eye doctor if your symptoms are frequent, persistent, worsening, or affecting daily life. You should also book an appointment if your eyes are red, sore, gritty, watery, blurry, or sensitive to light. - Are over-the-counter eye drops enough for dry eyes?
Over-the-counter drops may help mild dry eyes, but they may not treat the underlying cause. If your symptoms keep returning or drops are not working, an eye doctor can help identify what is really causing the problem. - Can dry eye be cured permanently?
Dry eye can often be managed very effectively, but it may not always be permanently cured. Some cases are temporary, while others need ongoing care with drops, eyelid treatment, environmental changes, or medical treatment.
Final Thoughts: Getting the Right Help for Dry Eyes
Dry eyes can affect far more than just comfort. When your eyes constantly feel irritated, watery, gritty, tired, or blurry, even simple daily activities like reading, driving, screen work, or wearing contact lenses can become frustrating. The important thing to remember is that dry eye is not always caused by the same issue. Some people struggle with reduced tear production, while others experience poor tear quality, eyelid gland problems, inflammation, allergies, or environmental triggers. This is why ongoing symptoms should not be ignored or treated with endless trial and error.
Seeing an eye doctor can help you understand what is actually causing your dry eye symptoms and which treatments are most suitable for your eyes. With the right diagnosis and personalised care plan, many people experience significant improvement in comfort and vision. If your symptoms are persistent, worsening, or affecting your quality of life, professional assessment is a sensible next step. If you’re considering seeing an eye doctor in London and want to know if it’s the right option, you’re welcome to reach out to us at Eye Clinic London to book a consultation.
References:
- Kojima, T. et al. (2013) Diagnostic Procedures and Management of Dry Eye, BioMed Research International, 2013, 1–18. Available at: https://pmc.ncbi.nlm.nih.gov/articles/PMC3760183
- Stern, M.E. et al. (2013) The pathology of dry eye: the interaction between the ocular surface and lacrimal glands, Cornea, 32, pp. S4–S8. Available at: https://academic.oup.com/cei/article/184/2/248/6412149
- O’Neil, E.C., Henderson, M., Massaro-Giordano, M. and Bunya, V.Y. (2019) Advances in dry eye disease treatment, Current Opinion in Ophthalmology, 30(3), pp. 166–178. Available at: https://pubmed.ncbi.nlm.nih.gov/30883442/
- Nebbioso, M. et al. (2017) Analysis of the Pathogenic Factors and Management of Dry Eye in Ocular Surface Disorders, International Journal of Molecular Sciences, 18(8), p. 1764. Available at: https://www.mdpi.com/1422-0067/18/8/1764
- Heidari, M. et al. (2019) Dry Eye Disease: Emerging Approaches to Disease Analysis and Therapy, Journal of Clinical Medicine, 8(9), p. 1439. Available at: https://www.mdpi.com/2077-0383/8/9/1439

