Will I Go Blind From Glaucoma? (Real Risk Explained Clearly)

Glaucoma is a condition that understandably causes anxiety because it is linked to vision loss. However, the most important thing to know is that blindness is not the typical outcome for most people today, especially when the condition is detected early and managed properly.
Glaucoma is a group of eye conditions that damage the optic nerve, often due to increased eye pressure. The key concern is that this damage is usually gradual and painless, which is why regular eye checks are so important. If left untreated, it can lead to progressive loss of peripheral vision and, in advanced cases, severe vision impairment.
The reassuring reality is that modern treatments are highly effective at slowing or stopping progression. These may include prescription eye drops, laser treatments, or surgical procedures aimed at lowering eye pressure and protecting the optic nerve. When managed consistently, most patients maintain useful vision throughout their lives and do not go blind.
The biggest factor in protecting your vision is early diagnosis and ongoing follow-up. When treatment is started at the right time and followed properly, the risk of significant vision loss is greatly reduced. While glaucoma is a lifelong condition, it is very often manageable with the right care and regular monitoring.
What Glaucoma Actually Is
Glaucoma refers to a group of eye conditions that damage the optic nerve, which is responsible for transmitting visual information from the eye to the brain. When this nerve becomes damaged over time, it can lead to gradual changes in vision.
One of the most common factors associated with glaucoma is increased intraocular pressure (pressure inside the eye). However, it is important to understand that glaucoma can also occur even when eye pressure is within a normal range, which makes it a more complex condition than many people realise.
Because glaucoma usually develops slowly and without obvious early symptoms, many individuals are unaware they have it in the initial stages. This is why it is often referred to as a “silent” eye condition, and regular eye examinations are essential for early detection and prevention of vision loss.
Why People Fear Blindness
The fear of blindness often comes from misunderstanding the condition and how it progresses. Glaucoma, if left untreated, can lead to gradual and irreversible vision loss. This is why it is often associated with more severe outcomes and why early awareness is so important. However, it is equally important to understand that blindness is not an inevitable outcome for most people with glaucoma.
- Risk comes mainly from untreated disease: Vision loss typically occurs in cases where glaucoma is not diagnosed or not managed properly. When left untreated, damage to the optic nerve can progress over time and affect vision.
- Early detection changes outcomes: With regular eye checks and early diagnosis, treatment can be started before significant damage occurs. This greatly reduces the risk of severe vision loss.
- Progression can often be controlled: Modern treatments, including eye drops, laser therapy, and surgery when needed, can slow or control the progression of glaucoma. Many patients are able to maintain useful vision throughout their lives.
- Fear often based on outdated understanding: A lot of anxiety around blindness comes from older information or extreme cases. Advances in modern eye care have significantly improved long-term outcomes for most patients.
Overall, while glaucoma is a serious condition, early detection and proper management mean that blindness is not a common or unavoidable outcome.
Types of Glaucoma
Glaucoma is not a single condition but a group of eye diseases, and different types can behave in very different ways. The most common type is open-angle glaucoma, which develops slowly over time. In this form, damage to the optic nerve progresses gradually, often without noticeable symptoms in the early stages.
Another important type is angle-closure glaucoma, which can occur suddenly when the drainage angle in the eye becomes blocked. This can lead to a rapid rise in eye pressure and may cause symptoms such as severe eye pain, headache, nausea, and sudden vision changes. Because it develops quickly, it is considered a medical emergency and requires urgent treatment.
There are also other less common forms of glaucoma, each with different causes and progression patterns. Because of these variations, understanding the specific type of glaucoma you have is essential for accurate risk assessment, appropriate treatment planning, and long-term protection of vision.
How Vision Is Affected
Glaucoma typically affects peripheral (side) vision first, which means early changes can be subtle and easy to miss. Because central vision is usually preserved in the early stages, many people do not notice any problems with their eyesight at the beginning.
As the condition progresses slowly over time, the brain can adapt to gradual vision loss, which further masks early symptoms. This is one of the main reasons glaucoma is often detected later than other eye conditions. In daily life, patients may unconsciously compensate without realising that their field of vision is narrowing.
Early detection is crucial because treatment is most effective at preventing further damage rather than reversing it. Regular eye examinations allow changes in eye pressure and optic nerve health to be identified early, helping to preserve vision and reduce the risk of significant long-term loss.
Can You Go Completely Blind?
Glaucoma can lead to vision loss if it is not diagnosed or properly treated, but complete blindness is relatively rare in modern practice. In most cases, severe vision loss only occurs when the condition has been left untreated for a long time or has progressed to an advanced stage.
With early diagnosis and consistent management, the progression of glaucoma can usually be slowed or even stabilised. Treatments such as eye drops, laser procedures, or surgery are designed to lower eye pressure and protect the optic nerve from further damage. Because of these advances, most patients are able to maintain useful vision throughout their lives.
While glaucoma is a lifelong condition that requires ongoing monitoring, the risk of total blindness has significantly decreased with modern care. With regular follow-ups and adherence to treatment, many people continue to live independently with preserved vision.
Importance of Early Detection
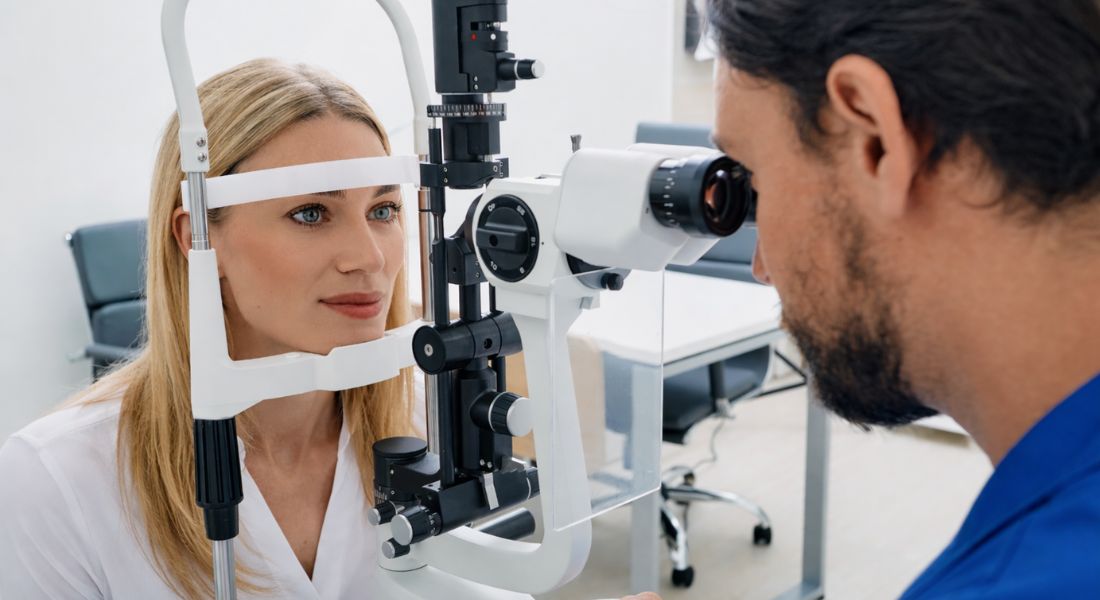
Glaucoma is a condition where early detection plays a crucial role in preserving vision. The earlier it is identified, the easier it is to manage and slow down its progression. Although any damage to the optic nerve cannot be reversed, timely treatment can significantly reduce the risk of further deterioration.
Routine eye examinations are essential because glaucoma often develops without noticeable symptoms in its early stages. Regular eye tests allow specialists to detect subtle changes in eye pressure and optic nerve health before significant vision loss occurs. In many cases, people are diagnosed during these routine checks even before they experience any visual problems.
Starting treatment early helps protect long-term vision and maintain quality of life. With proper monitoring and management, progression can often be controlled effectively, reducing the likelihood of serious vision impairment in the future.
Role of Eye Pressure
Glaucoma is closely linked to intraocular pressure (eye pressure), which is one of the most important risk factors in the condition. When eye pressure is too high, it can gradually damage the optic nerve, leading to progressive vision loss over time. However, it is important to understand that not all individuals with glaucoma have elevated eye pressure, which is why the condition can be complex and vary from person to person.
The primary goal of treatment is to lower and control eye pressure to a safe level for the individual. This helps slow or stop further damage to the optic nerve and reduces the risk of ongoing vision loss. Treatments may include eye drops, laser therapy, or surgical procedures, depending on the severity and type of glaucoma.
Regular monitoring is essential, as eye pressure can change over time. Consistent check-ups allow adjustments to treatment when needed, ensuring that pressure remains well controlled. By maintaining stable eye pressure, long-term vision can be better protected and disease progression can often be significantly slowed.
How Glaucoma Is Diagnosed
Glaucoma is diagnosed using a combination of tests that assess different aspects of eye health. These tests help identify early signs of the condition and monitor any changes over time. They are generally quick, painless, and can be done during a routine eye examination. Because glaucoma can progress slowly without obvious symptoms, regular testing is essential for early detection and ongoing management.
- Eye pressure measurement (tonometry): This test measures the pressure inside your eye. Increased intraocular pressure can be a risk factor for glaucoma, although it is not the only indicator.
- Optic nerve assessment: The optic nerve is carefully examined to check for any signs of damage. Changes in the optic nerve can indicate the presence or progression of glaucoma.
- Visual field testing: This test checks your peripheral (side) vision. It helps detect any areas of vision loss and is important for tracking how glaucoma may be affecting your sight over time.
- Ongoing monitoring over time: These tests are often repeated regularly to monitor any changes. This allows your eye specialist to detect progression early and adjust treatment if needed.
- Guiding treatment decisions: Accurate diagnosis and consistent monitoring are essential for creating an effective treatment plan. The results of these tests help determine the most appropriate management approach.
Overall, glaucoma diagnosis relies on a combination of simple, non-invasive tests that provide a clear picture of eye health and help guide long-term care.
Treatment Goals
Glaucoma treatment is focused primarily on preserving existing vision rather than restoring vision that has already been lost. The main objective is to slow down or stop the progression of optic nerve damage so that further vision loss can be prevented or minimised.
Management of glaucoma is typically long-term and requires ongoing consistency with treatment and regular monitoring. This may include the continued use of prescribed eye drops, laser procedures, or surgical interventions depending on the individual case. Staying adherent to treatment plays a key role in maintaining stable eye health.
While glaucoma cannot be cured or reversed, modern treatment approaches are highly effective at controlling the condition in most patients. The overall goal is stability keeping eye pressure under control and protecting remaining vision for as long as possible to maintain quality of life.
Eye Drops as First Treatment

Glaucoma is most commonly treated initially with medicated eye drops, which are designed to lower intraocular pressure. By reducing this pressure, the drops help to decrease strain on the optic nerve and slow the progression of damage over time. This makes them an important first-line option in many treatment plans.
Eye drops are usually prescribed for daily use, and they must be used consistently to be effective. They work best when taken at the same time each day, as this helps maintain stable eye pressure control. Regular use is essential because inconsistent application can reduce their overall effectiveness.
Missing doses or using drops irregularly can allow eye pressure to fluctuate, which may increase the risk of further optic nerve damage. This is why adherence to the prescribed routine is so important in long-term management. Even small lapses in treatment can affect overall disease control.
Although simple in form, eye drops are a highly effective and widely used treatment option. When used correctly and combined with regular monitoring, they play a key role in preserving vision and maintaining long-term eye health.
Laser Treatment Options
Glaucoma can sometimes be managed with laser treatments, depending on the type and severity of the condition. Laser procedures are designed to improve the drainage of fluid from the eye, which helps reduce intraocular pressure. By lowering this pressure, the risk of further optic nerve damage can be decreased.
Laser treatment is generally quick and minimally invasive, often performed as an outpatient procedure. Most patients can return to normal activities shortly afterwards, although some may experience mild temporary side effects such as blurred vision or irritation. The exact results can vary depending on the individual and the specific type of glaucoma being treated.
In some cases, laser treatment may reduce the need for long-term use of eye drops or help delay the need for surgery. However, it is not a permanent cure and ongoing monitoring is still required. Overall, laser therapy is a useful and effective option in the management of glaucoma for many patients.
Surgical Treatments
In more advanced cases of glaucoma, surgical treatment may be recommended when eye drops or laser treatments are not enough to control eye pressure effectively. The main aim of surgery is to improve fluid drainage from the eye, which helps reduce intraocular pressure and protect the optic nerve from further damage. Surgical options are carefully considered and tailored to each patient’s condition.
- Creating new drainage pathways: Glaucoma surgery works by improving or creating new routes for fluid to drain from the eye. This helps lower pressure and reduces the risk of ongoing optic nerve damage.
- Effective pressure reduction: By improving fluid outflow, surgery can significantly lower eye pressure, especially in cases where other treatments have not achieved sufficient control.
- Generally safe and well-established procedures: Modern glaucoma surgeries are widely performed and considered safe when carried out by experienced specialists. As with any surgery, there are risks, but these are carefully managed.
- Used when other treatments are insufficient: Surgery is typically recommended only when medications or laser treatments are no longer effective in controlling the condition adequately.
- Careful post-operative monitoring: After surgery, regular follow-up appointments are essential to ensure proper healing, monitor eye pressure, and check that the treatment is working as expected.
Overall, glaucoma surgery provides an important long-term option for controlling eye pressure and protecting vision in more advanced or difficult-to-manage cases.
How Treatment Prevents Blindness
Glaucoma treatment focuses on protecting the optic nerve from ongoing damage. By lowering intraocular pressure, treatment reduces the stress placed on the nerve fibres inside the eye. This helps slow down or stop the progression of vision loss over time.
When the condition is diagnosed early and managed consistently, most patients are able to maintain useful vision and avoid severe stages of the disease. Modern treatments, including eye drops, laser therapy, and surgery when needed, are highly effective in controlling eye pressure. As a result, significant vision impairment is much less common than in the past.
The key principle in preventing blindness is early and continuous management. Regular monitoring ensures that treatment remains effective and can be adjusted if needed. With proper care and adherence to treatment, the risk of severe vision loss is greatly reduced.
Importance of Consistency
Glaucoma management depends heavily on consistency in both treatment and monitoring. Medications and prescribed therapies must be followed daily, as regular use helps maintain stable eye pressure and reduces the risk of ongoing optic nerve damage. Skipping doses or using treatment inconsistently can lead to fluctuations in pressure, which may increase the risk of progression.
Regular check-ups are equally important in long-term care. These appointments allow eye specialists to track changes in eye pressure, assess optic nerve health, and determine whether the current treatment plan is working effectively. Over time, adjustments may be made to ensure optimal control of the condition.
Consistency is one of the most important factors in protecting vision. When patients adhere closely to treatment and attend scheduled follow-ups, the risk of significant vision loss is greatly reduced. This steady and ongoing approach helps maintain long-term eye health and stability.
Monitoring Progress
Glaucoma is a long-term condition that requires regular monitoring to track its progression over time. This typically includes routine eye pressure measurements as well as detailed vision tests to assess both central and peripheral vision. These assessments help provide a clear picture of how the condition is developing.
By carefully tracking changes, doctors can identify whether the current treatment plan is working effectively or whether adjustments are needed. Early detection of any progression allows for timely intervention, which is essential in preventing further optic nerve damage. This makes ongoing monitoring a key part of effective glaucoma management.
Because glaucoma can change gradually, regular check-ups are essential even when symptoms are not noticeable. Consistent follow-up appointments ensure that any subtle changes are detected early, helping to maintain stable vision and reduce the risk of long-term vision loss.
Lifestyle Factors
Lifestyle habits can play a supportive role in maintaining overall eye health and general well-being, especially for people managing glaucoma. While healthy choices cannot replace medical treatment, they can complement it and contribute to better long-term health outcomes. A balanced lifestyle may help support both physical and eye health.
- Healthy habits and general well-being: Regular exercise, a balanced diet, and good overall health can support the body’s systems, including the eyes. While these habits do not treat glaucoma directly, they contribute to overall wellness.
- Stress management: Managing stress can be beneficial for general health and may help you feel more comfortable in managing a long-term condition. Relaxation techniques and a balanced routine can support emotional well-being.
- Eye protection and care: Protecting your eyes from injury and following regular eye check-ups is important. Wearing appropriate eye protection in risky environments can help prevent avoidable damage.
- Support alongside medical treatment: Lifestyle improvements should be seen as supportive measures rather than replacements for prescribed treatment. They work best when combined with regular medical care and follow-up.
Overall, a healthy lifestyle can support your treatment plan and contribute to better overall health, but ongoing medical management remains the most important factor in controlling glaucoma.
Genetic Factors
Glaucoma can sometimes have a genetic component, meaning that family history plays an important role in determining risk. If a close family member has glaucoma, your likelihood of developing the condition may be higher compared to the general population. However, having a family history does not mean you will definitely develop glaucoma.
Because of this increased risk, regular eye screening becomes especially important for individuals with a family history of the condition. Early and routine examinations allow eye specialists to detect subtle changes before symptoms appear. This early identification is crucial in preventing or slowing down disease progression.
While genetics can influence susceptibility, they do not determine the final outcome. With timely diagnosis and proper management, glaucoma can often be controlled effectively. This means that even those at higher genetic risk can significantly reduce their chances of serious vision loss through regular monitoring and early intervention.
Age and Risk
Glaucoma becomes more common as people get older, with risk increasing significantly after the age of 40. This is because age-related changes in the eye can affect fluid drainage and increase susceptibility to optic nerve damage over time. As a result, older adults are generally considered at higher risk compared to younger individuals.
Because of this increased risk, regular eye examinations become especially important with advancing age. Routine screening helps detect early signs of glaucoma before noticeable vision loss occurs. Early monitoring allows for timely intervention, which can greatly improve long-term outcomes.
Age is one of the most significant risk factors for glaucoma, but it does not guarantee that the condition will develop. With consistent eye checks and early detection, age-related risk can be managed effectively. Preventive care and ongoing monitoring remain essential for protecting vision throughout life.
Symptoms You Should Not Ignore
Glaucoma is often called a “silent” condition because in its early stages it usually does not produce noticeable symptoms. Many people do not realise they have it until vision changes begin to develop gradually over time. When symptoms do appear in later stages, they often involve loss of peripheral (side) vision rather than central vision.
In some cases, particularly with angle-closure glaucoma, symptoms can appear suddenly and become severe. These may include intense eye pain, headache, blurred vision, nausea, or seeing halos around lights. This type of presentation is a medical emergency and requires immediate treatment to prevent rapid vision loss.
Because early stages are often symptom-free, it is very important not to ignore any changes in vision. Even subtle or temporary visual disturbances should be checked by an eye specialist. Prompt attention to symptoms helps ensure early diagnosis and reduces the risk of permanent vision damage.
Emotional Impact of Diagnosis
Glaucoma can have a significant emotional impact when first diagnosed, as many people immediately associate it with vision loss or blindness. It is very common to feel worried, anxious, or overwhelmed, especially because the condition is lifelong and requires ongoing care. These emotional reactions are completely normal and understandable.
However, gaining a clear understanding of the condition often helps reduce fear. When patients learn how glaucoma progresses slowly and how effectively it can be managed with modern treatments, their confidence usually improves. Knowing that most people retain useful vision with proper care can be reassuring.
Support from healthcare professionals, family, and patient resources also plays an important role. Education helps patients feel more in control of their condition and reduces uncertainty. With the right information and guidance, many people are able to cope well and manage glaucoma with confidence over the long term.
Long-Term Outlook
Most people with glaucoma are able to maintain useful vision throughout their lives, especially when the condition is diagnosed early and managed appropriately. With consistent treatment and regular monitoring, progression is often slow, allowing many patients to continue living normal and independent lives. The long-term outlook depends greatly on early detection and ongoing care.
- Slow progression with treatment: When glaucoma is well controlled, vision loss typically progresses very slowly. Treatment helps protect the optic nerve and maintain stable vision for many years.
- Importance of regular care: Ongoing eye checks are essential to monitor eye pressure and detect any changes early. This allows treatment to be adjusted if needed to maintain control of the condition.
- Better outcomes with early diagnosis: Detecting glaucoma early significantly improves long-term results. Starting treatment at an early stage helps preserve vision and reduce the risk of significant damage.
- Possibility of long-term stability: With proper management, many patients experience long periods of stable vision without major changes, supporting a good quality of life.
Overall, while glaucoma is a lifelong condition, the long-term outlook is often positive when it is properly treated and regularly monitored.
Importance of Specialist Care
Glaucoma management requires specialist care because it is a complex, long-term condition that affects vision gradually. Ophthalmologists are trained to assess eye pressure, optic nerve health, and visual field changes in detail, allowing them to create precise and individualised treatment plans. This level of expertise helps ensure that the condition is managed as effectively as possible.
Regular follow-ups with an eye specialist are essential for tracking disease progression over time. During these visits, treatment may be adjusted based on changes in eye pressure or vision tests. This proactive approach helps maintain better control of the condition and reduces the risk of further optic nerve damage.
Expert care plays a crucial role in both safety and long-term outcomes. With specialist supervision, patients receive timely interventions and more accurate monitoring, which significantly improves the chances of preserving vision.
Advances in Treatment
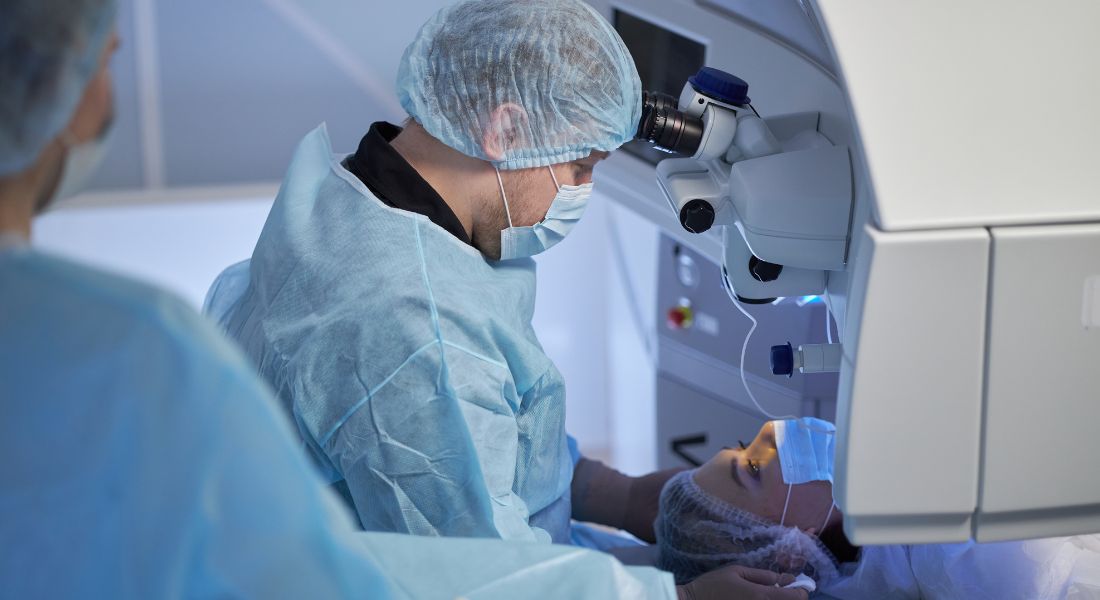
Glaucoma treatment has improved significantly in recent years due to advances in medical technology and research. Modern diagnostic tools allow earlier detection of optic nerve damage, which helps clinicians begin treatment sooner and slow disease progression more effectively. As a result, long-term outcomes for many patients are better than in the past.
Newer medications and laser therapies have also expanded treatment options for controlling intraocular pressure. These treatments are often more targeted and better tolerated, helping patients manage the condition with greater ease and consistency. In addition, surgical techniques have become safer and more precise, offering improved outcomes for more advanced cases.
Overall, glaucoma care continues to evolve, with ongoing research leading to more effective and personalised approaches. These advancements are helping reduce the risk of severe vision loss and improving quality of life for patients living with the condition.
Individual Risk Variation
Glaucoma does not progress in the same way for every patient, as the condition can vary widely in severity, speed of progression, and response to treatment. Some individuals experience very slow changes over many years, while others may have a more rapid progression that requires closer monitoring and more intensive management.
Because of this variation, individual assessment is essential in every case. Eye specialists evaluate factors such as eye pressure, optic nerve appearance, visual field changes, age, and overall health to determine each patient’s specific risk level. This allows for a more accurate understanding of how the disease is likely to behave over time.
Treatment is always personalised based on these findings. Some patients may only need mild pressure control, while others may require stronger medications, laser therapy, or surgical intervention. Since no two cases of glaucoma are exactly the same, tailored care ensures the best possible protection of vision for each individual.
Can Vision Loss Be Reversed?
Glaucoma causes damage to the optic nerve, and unfortunately, this damage cannot be reversed once it has occurred. The optic nerve does not regenerate, which means any vision loss that has already happened is usually permanent. This is why early detection and timely treatment are so important in managing the condition.
However, while existing vision loss cannot be restored, further deterioration can often be prevented or significantly slowed with proper treatment. Lowering eye pressure through medications, laser procedures, or surgery helps stabilise the condition and protect the remaining healthy vision. This makes ongoing management a key part of care.
The main focus of glaucoma treatment is therefore prevention rather than reversal. By controlling progression early and consistently, many patients are able to maintain useful vision and avoid severe impairment over time.
Importance of Early Action
Acting early is one of the most important factors in managing glaucoma effectively. When the condition is detected and treated in its early stages, treatment tends to work better and can significantly slow or prevent further damage to vision. Early intervention focuses on protecting vision before permanent changes occur.
- Better treatment effectiveness in early stages: In the early stages of glaucoma, the optic nerve is less damaged, which means treatments are often more effective at controlling eye pressure and slowing progression.
- Prevention of long-term progression: Starting treatment early helps reduce the risk of ongoing damage. This can preserve vision for much longer and maintain overall visual function.
- Risks of delaying care: Delaying diagnosis or treatment can allow the condition to progress silently. Since glaucoma often has no obvious early symptoms, damage may occur before it is noticed.
- Protection of long-term vision: Early intervention plays a key role in protecting sight. The sooner treatment begins, the better the chances of maintaining stable vision over time.
Overall, early action is essential in glaucoma care. Timely diagnosis and treatment significantly improve outcomes and help preserve vision for the long term.
Regular Eye Tests
Glaucoma is often detected through routine eye examinations because it typically develops without obvious early symptoms. Regular eye tests allow eye care professionals to identify subtle changes in eye pressure, optic nerve health, and vision before noticeable damage occurs. This makes screening one of the most important tools for early detection.
Even if a person feels their vision is normal, regular check-ups are still essential. Many cases of glaucoma are discovered during standard eye exams before the patient is aware of any problem. Early diagnosis at this stage allows treatment to begin sooner, which significantly improves long-term outcomes.
Prevention of vision loss largely depends on consistent screening and monitoring. By attending routine eye tests, patients increase the chances of catching glaucoma early and managing it effectively. This is why regular eye examinations are considered vital for protecting long-term eye health.
Support for Patients
Glaucoma can feel overwhelming at first, but strong support systems are available to help patients manage the condition with confidence. Education plays a key role in reducing fear, as understanding how the condition progresses and how it is treated often helps patients feel more reassured and less anxious.
Eye care professionals typically take time to explain the diagnosis, treatment options, and long-term management plan in a clear and supportive way. This open communication helps patients feel more involved in their care and gives them a greater sense of control over their condition. As a result, adherence to treatment and follow-up appointments often improves.
In addition to medical guidance, emotional and practical support from healthcare teams, family, and patient resources can make a significant difference. Knowing that glaucoma is a manageable condition for most people helps reduce isolation and builds confidence in long-term care.
Managing Expectations
Glaucoma requires long-term management, and it is important for patients to have a clear understanding of what treatment can realistically achieve. While current therapies cannot restore vision that has already been lost due to optic nerve damage, they are highly effective in slowing or stopping further progression of the disease. This makes early and consistent treatment essential for preserving remaining sight.
Having realistic expectations is an important part of successful long-term care. The main goal of treatment is not to cure glaucoma, but to maintain stable vision and prevent further deterioration. When patients understand this, they are often better able to accept the treatment process and remain committed to ongoing care.
Clear understanding of the condition also helps improve confidence and reduces anxiety. Knowing that stability is the primary aim of treatment allows patients to focus on protecting their vision over time, leading to better satisfaction and adherence to their management plan.
FAQs:
- Will I definitely go blind if I have glaucoma?
No, most people with glaucoma do not go blind. With early diagnosis and proper treatment, the condition can usually be controlled. The goal of treatment is to slow or stop progression rather than reverse damage. Many patients maintain useful vision for life. - What causes vision loss in glaucoma?
Vision loss happens when the optic nerve becomes damaged, often due to increased eye pressure. This damage affects how visual signals are sent to the brain. It usually starts with peripheral vision before affecting central vision. Without treatment, this damage can gradually worsen. - Can glaucoma-related blindness be prevented?
Yes, in most cases blindness can be prevented with early detection and consistent treatment. Eye drops, laser therapy, or surgery help lower eye pressure and protect the optic nerve. Regular monitoring is essential to prevent progression. The earlier it is treated, the better the outcome. - Is glaucoma treatable?
Yes, glaucoma is treatable but not curable. Treatment focuses on controlling eye pressure to prevent further damage. This may include eye drops, laser treatment, or surgery depending on severity. With proper care, most patients can manage the condition effectively. - Does glaucoma cause sudden blindness?
Most types of glaucoma cause slow, gradual vision loss rather than sudden blindness. However, angle-closure glaucoma can develop suddenly and requires urgent treatment. If treated quickly, vision can often be saved. Regular eye checks help prevent unexpected complications. - How often should I have eye tests if I have glaucoma?
Most patients need regular follow-up every few months, depending on severity. These visits include eye pressure checks and vision tests. Monitoring helps ensure treatment is working effectively. Your eye specialist will recommend the right schedule for you. - Can glaucoma be stopped from getting worse?
Yes, treatment can often slow or stop progression. While existing damage cannot be reversed, further loss can usually be prevented. Consistent use of medication is very important. Ongoing monitoring ensures treatment remains effective. - What are the early warning signs of glaucoma?
Early glaucoma often has no symptoms, which is why it is called a silent condition. Some people may notice gradual peripheral vision loss. In rare cases, eye pain or blurred vision can occur. Routine eye exams are the best way to detect it early. - Who is most at risk of going blind from glaucoma?
People who are diagnosed late or do not follow treatment are at higher risk. Advanced cases without proper management can lead to significant vision loss. Age, family history, and high eye pressure also increase risk. Early and consistent care greatly reduces the chance of blindness. - Can I live a normal life with glaucoma?
Yes, most people with glaucoma continue to live normal, independent lives. With treatment, vision can often be preserved for many years. Adjustments may be needed in advanced cases, but daily activities are usually unaffected. Proper management is key to maintaining quality of life.
Final Thoughts: Protecting Your Vision with Early and Consistent Glaucoma Care
Glaucoma can feel worrying at first, especially because it is often linked with the fear of blindness. However, modern understanding of the condition shows that vision loss is not inevitable. With early diagnosis and regular monitoring, the disease can usually be controlled effectively. Most patients are able to maintain useful vision throughout their lives.
The key factor in preventing progression is consistency with treatment and follow-up care. Eye drops, laser procedures, or surgery are used to lower eye pressure and protect the optic nerve. While these treatments cannot reverse existing damage, they are highly effective at preventing further loss. Staying committed to your treatment plan makes a significant difference over time. If you’d like to find out whether glaucoma treatment in London is suitable for you, feel free to contact us at Eye Clinic London to arrange a consultation.
References:
- Azuara-Blanco, A., Burr, J., Ramsay, C., Cooper, D., Foster, P.J. and Friedman, D.S., 2016. Effectiveness of early lens extraction for the treatment of primary angle-closure glaucoma (EAGLE study). The Lancet, 388(10052), pp.1389-1397. https://pubmed.ncbi.nlm.nih.gov/27707497/
- Sun, X., Dai, Y., Chen, Y., Yu, D., Cringle, S.J. and Yu, P.K., 2017. Primary angle closure glaucoma: What we know and what we don’t know. Progress in Retinal and Eye Research, 57, pp.26-45. https://pmc.ncbi.nlm.nih.gov/articles/PMC5337134/
- Tham, Y.C., Li, X., Wong, T.Y., Quigley, H.A., Aung, T. and Cheng, C.Y., 2014. Global prevalence of glaucoma and projections of glaucoma burden through 2040. Ophthalmology, 121(11), pp.2081-2090. https://pubmed.ncbi.nlm.nih.gov/24974815/
- Wang, Y., Yan, L., Qin, Y. and Fan, F., 2025. Research progress of corneal characteristics and changes in primary angle-closure glaucoma. Biomedical Reports, 22(4), p.59. https://pmc.ncbi.nlm.nih.gov/articles/PMC11843189/
- Aiad, A., 2025. Acute angle-closure glaucoma as an ocular complication of dengue fever: A comprehensive review. Cureus, 17(4), e82119. https://pubmed.ncbi.nlm.nih.gov/40357076/

