Can You Have ICL Surgery If You Have Rheumatoid Arthritis or Autoimmune Disease?
If you have an autoimmune condition such as rheumatoid arthritis, it’s natural to question whether ICL surgery is a safe option for you. These conditions can influence inflammation, healing, and overall eye health, all of which play an important role in surgical outcomes. Understanding how your condition may interact with the procedure can help you feel more informed and confident when considering your options.
ICL surgery is a highly effective method of vision correction that involves placing a lens inside your eye rather than reshaping the cornea. This can be particularly beneficial if your corneas are not suitable for laser procedures. However, autoimmune conditions often require a more detailed and cautious evaluation before surgery is recommended. Your surgeon will look closely at your medical history, current treatment, and disease activity.
The reassuring news is that many people with well-controlled autoimmune diseases can still be suitable candidates for ICL surgery. The most important factors are stability of your condition, proper management of inflammation, and careful preoperative assessment. With personalised planning and close collaboration between your eye specialist and healthcare provider, you can safely explore whether this procedure is right for you.
What Are Autoimmune Diseases?
Autoimmune diseases occur when your immune system mistakenly attacks your own body’s tissues instead of protecting them. Conditions such as rheumatoid arthritis, lupus, and other similar disorders can affect different parts of your body, including your joints, skin, and even your eyes. Because these conditions vary widely, the way they affect your overall health can be different from one person to another. Understanding this basic concept helps you see why extra care is needed when considering surgery.
These conditions are often linked with ongoing or chronic inflammation within the body. This inflammation can influence how your body responds to surgical procedures and how effectively you heal afterwards. In some cases, it may slow the healing process or increase sensitivity in the eyes. This is why your surgeon will take a detailed look at your medical history before recommending treatment.
Understanding your specific autoimmune condition is the first step in deciding whether ICL surgery is suitable for you. Your healthcare team will assess how stable your condition is and whether it is well controlled. By gaining a clear picture of your overall health, they can guide you towards the safest and most effective treatment option.
Understanding Rheumatoid Arthritis and the Eyes
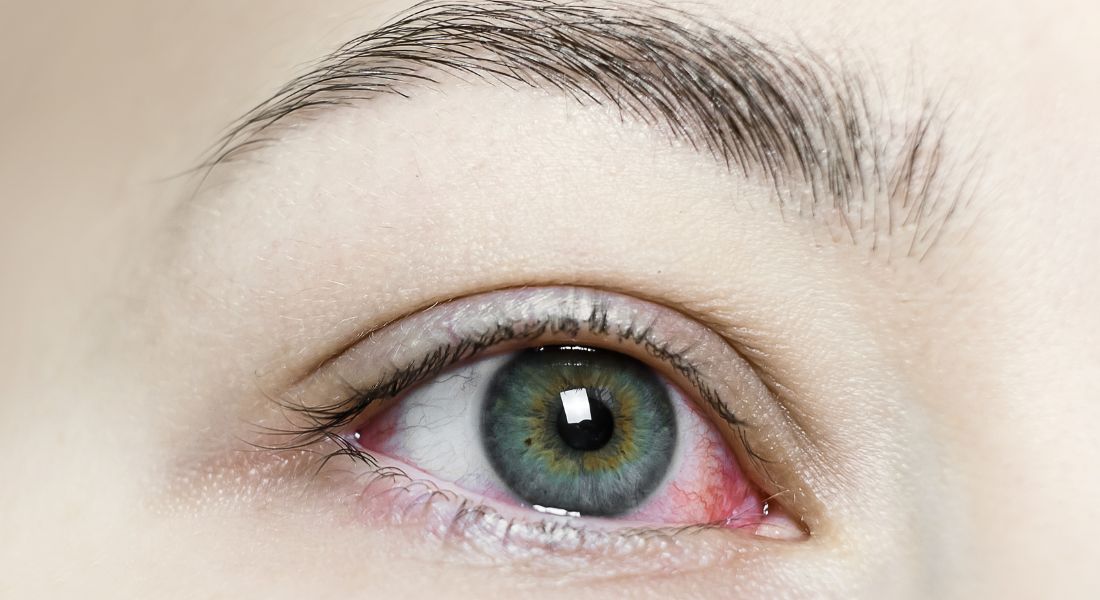
Rheumatoid Arthritis doesn’t just affect your joints it can also have an impact on your eyes. You might notice symptoms such as dryness, irritation, or even inflammation. These changes can influence how comfortable your eyes feel and how well they respond to treatment. Understanding this connection helps ensure that any vision correction procedure is planned with your overall eye health in mind.
- Dry eye symptoms: You may experience dryness, a gritty feeling, or sensitivity to light. This happens because rheumatoid arthritis can reduce tear production. Dryness is important to manage, as it can affect your comfort both during and after surgery.
- Inflammation in the eye: In some cases, the condition can lead to inflammation, such as scleritis or uveitis. These conditions need to be carefully monitored and controlled before considering any surgical procedure.
- Impact on healing and recovery: Autoimmune conditions like rheumatoid arthritis can sometimes slow healing. Your surgeon will take this into account when planning your treatment and recovery timeline.
- Adjustments in surgical planning: If dryness or inflammation is present, your treatment plan may include managing these issues first. This helps create the best possible conditions for a safe and successful procedure.
Before recommending surgery, your eye specialist will carry out a thorough assessment to understand how rheumatoid arthritis is affecting your eyes. By addressing any underlying issues in advance, you can move forward with greater confidence and a better chance of achieving a comfortable, successful outcome.
What Is ICL Surgery?
ICL surgery involves placing a small, flexible lens inside your eye to improve your vision. This lens sits behind the iris and works alongside your natural lens to focus light more accurately onto the retina. Because it complements your existing eye structure rather than replacing it, the procedure feels more natural for many patients. Understanding how the lens functions can help you feel more at ease about the process.
The procedure itself is minimally invasive and typically quick, with most treatments completed in a short time. One of its key advantages is that it is reversible, meaning the lens can be removed or replaced if needed in the future. Many patients experience high-quality visual outcomes, often with sharper clarity than glasses or contact lenses. This makes ICL surgery a popular option for people seeking long-term vision correction.
For individuals with autoimmune conditions, the fact that ICL does not reshape the cornea can be particularly beneficial. This approach may reduce certain risks associated with healing and surface inflammation. However, careful evaluation is still essential to ensure your condition is stable and suitable for surgery. Your surgeon will assess your overall health to determine whether this option is right for you.
Is Autoimmune Disease a Contraindication?
Having an autoimmune disease does not automatically mean you cannot have ICL surgery. Many patients with conditions such as rheumatoid arthritis or lupus undergo the procedure successfully and achieve excellent visual outcomes. The key factor is not simply the diagnosis, but how well your condition is managed. When your health is stable, surgery can often be considered safely.
However, if your condition is active or poorly controlled, the risks may be higher. Ongoing inflammation can affect how your eyes respond to surgery and may slow down the healing process. In some cases, this could lead to increased discomfort or a higher chance of complications. This is why careful timing and preparation are so important.
Your surgeon will assess your suitability based on the stability of your condition and your overall eye health. They may also work closely with your healthcare provider to understand your medical history and current treatment. By taking a personalised approach, they can determine whether it is safe to proceed or if it is better to wait until your condition is more controlled.
Importance of Disease Stability
Stability is one of the most important factors when deciding whether ICL surgery is safe for you. If your autoimmune condition is well controlled, your body is more likely to respond positively to the procedure. This reduces the risk of complications and supports a smoother healing process. A stable condition gives your surgeon greater confidence in recommending treatment.
On the other hand, frequent flare-ups or recent changes in your medication may suggest that your condition is not yet stable. During these periods, your immune system may be more reactive, which can increase inflammation and affect healing. In such situations, your surgeon may advise postponing surgery until your condition is better managed. This cautious approach helps protect your long-term eye health.
When your condition is stable, your body can respond more predictably to surgery. Healing tends to be more consistent, and the chances of achieving a successful outcome are higher. Your healthcare team will work with you to ensure the timing is right, so you can proceed with confidence and minimise unnecessary risks.
Inflammation and Healing
Autoimmune conditions are closely linked to inflammation within the body. This underlying inflammation can influence how your eyes respond after surgery and how efficiently they heal. When inflammation levels are higher than normal, your body may take longer to recover. Understanding this connection helps explain why careful planning is essential before proceeding with ICL surgery.
Increased inflammation can sometimes lead to a slower recovery or temporary discomfort after the procedure. You might notice prolonged dryness, sensitivity, or mild irritation while your eyes adjust. Although these effects are usually manageable, they can be more noticeable if your condition is not well controlled. This is why managing inflammation before surgery plays such an important role.
Your surgeon may work closely with your specialist to ensure your condition is well controlled before going ahead. This coordinated approach helps reduce risks and supports a smoother healing process. By optimising your health beforehand, you improve your chances of a comfortable recovery and a successful visual outcome.
Dry Eye Considerations
Dry eye is quite common if you have an autoimmune condition, and it can affect both how your eyes feel and how clearly you see. You might notice irritation, a gritty sensation, or fluctuating vision throughout the day. While this doesn’t usually prevent you from having surgery, it does need to be properly managed beforehand to ensure the best possible outcome.
- Understanding your symptoms: Your specialist will ask about dryness, irritation, or blurred vision. They may also carry out simple tests to assess tear production and the quality of your tear film.
- Preparing the eye surface: Before surgery, the focus is on improving the health of the eye surface. This helps the eye respond better to treatment and supports smoother healing afterwards.
- Use of lubricating treatments: You may be advised to use lubricating eye drops or other treatments to keep your eyes comfortable. These help reduce dryness and protect the surface of the eye.
- Monitoring after the procedure: Even though ICL surgery does not usually worsen dry eye, your eyes will still be monitored closely after the procedure to ensure symptoms remain under control.
By managing dry eye properly before surgery, you can improve both comfort and visual quality afterwards. Taking these steps in advance helps create the best possible conditions for a smooth recovery and long-term eye health.
Medication and Immune Response
Many people with autoimmune conditions take medications that affect how the immune system works. These treatments, including immunosuppressants or anti-inflammatory drugs, help control disease activity but can also influence how your body heals after surgery. Because your immune response may be altered, there can be a slightly increased risk of slower healing or infection. Understanding this helps you see why extra care is taken before proceeding.
Your surgeon will carefully review your medication history as part of the preoperative assessment. They will consider the type of medication you are taking, the dosage, and how stable your condition has been. In some cases, adjustments to your treatment plan may be discussed with your physician before surgery. This ensures that any changes are safe and do not affect your overall health.
By coordinating your care, your medical team can prepare your body for the best possible surgical outcome. The goal is to maintain good control of your autoimmune condition while also supporting proper healing. With the right balance, you can approach the procedure with confidence, knowing that every precaution has been taken to protect your eye health.
Risk of Infection
If you take immune-suppressing medication for an autoimmune condition, there may be a slightly increased risk of infection after surgery. These medications reduce your body’s natural defence mechanisms, which can affect how it responds to bacteria. While this risk is generally low, it is an important factor your surgeon will consider before recommending ICL surgery. Understanding this helps you take the right precautions during recovery.
Strict hygiene and careful post-operative care play a key role in minimising this risk. You will be advised to use prescribed eye drops, keep your eyes clean, and avoid touching or rubbing them during the healing period. Following these instructions closely helps protect your eyes and supports a smooth recovery. Your clinical team will guide you through each step so you feel confident in your aftercare routine.
With proper precautions and careful monitoring, complications remain uncommon. Most patients recover without any serious issues, even when taking immune-modifying medications. Regular follow-up appointments allow your surgeon to detect and manage any concerns early. By staying consistent with your care plan, you can reduce risks and focus on achieving the best possible visual outcome.
Pre-Surgical Assessment

Before going ahead with ICL surgery, you will have a comprehensive eye examination to assess your suitability. This includes checking your overall eye health, measuring your prescription, and examining structures such as the cornea, lens, and retina. Your tear film may also be evaluated, as it plays an important role in comfort and healing after the procedure. These detailed checks help ensure your eyes are ready for surgery.
If you have an autoimmune condition, additional assessments may be needed to gain a clearer picture of your eye health. Your surgeon may look more closely at signs of inflammation, dryness, or any underlying issues that could affect healing. In some cases, they may also coordinate with your specialist to understand how stable your condition is. This extra level of evaluation helps reduce risks and improves overall outcomes.
A thorough pre-surgical assessment ensures that the procedure is both safe and appropriate for you. By identifying any potential concerns in advance, your surgeon can plan the surgery more precisely or recommend delaying it if needed. This careful approach allows you to move forward with confidence, knowing that your treatment has been tailored to your individual needs.
Corneal Health Evaluation
Even though ICL surgery doesn’t reshape your cornea, its overall health still plays an important role in your safety and visual outcome. If you have an autoimmune condition, your cornea may be more sensitive or slightly slower to heal. That’s why your surgeon will take extra care to assess its condition before recommending surgery.
- Checking corneal structure and thickness: Your surgeon will measure the shape and thickness of your cornea to make sure it is strong and stable. This helps confirm that your eye can safely support the procedure.
- Assessing corneal sensitivity: Autoimmune conditions can sometimes reduce corneal sensitivity. This can affect how your eye responds to dryness or healing, so it’s an important factor to evaluate.
- Looking for surface irregularities: The surface of your cornea will be examined for any signs of damage, inflammation, or dryness. A healthy surface is essential for comfort and clear vision after surgery.
- Treating any underlying issues first: If any concerns are found, such as dryness or minor surface problems, these will be managed before moving forward. This helps create the best possible conditions for surgery.
By carefully assessing your corneal health in advance, your surgeon can make sure your eyes are well prepared. This thorough approach helps reduce risks, improve comfort, and support a smooth recovery after your procedure.
Retinal and Internal Eye Health
The health of your retina and internal eye structures plays a vital role in determining whether ICL surgery is suitable for you. The retina is responsible for processing light and sending visual signals to your brain, so any underlying issues can affect your final visual outcome. In some cases, autoimmune conditions may involve deeper layers of the eye, making careful evaluation even more important. Understanding this helps you see why thorough testing is essential before surgery.
To assess this, your surgeon will use advanced imaging techniques to examine the inside of your eye in detail. These scans can detect subtle changes or early signs of problems that may not be noticeable during a routine eye exam. By identifying any concerns early, your surgeon can decide whether it is safe to proceed or if further management is needed first. This step adds an extra layer of safety to the decision-making process.
Ensuring that your internal eye health is stable helps reduce the risk of complications during and after surgery. When the retina and other internal structures are healthy, your eyes are better prepared to respond to the procedure and recover smoothly. This careful assessment allows your treatment to be planned with precision, giving you the best possible chance of achieving clear and stable vision.
Benefits of ICL for Autoimmune Patients
ICL surgery offers a number of advantages, particularly if you have an autoimmune condition affecting the surface of your eyes. Because the procedure does not reshape the cornea, it can be a more suitable option if you experience dry eye or surface-related sensitivity. This approach helps preserve the natural structure of your eye, which may reduce irritation during recovery. For many patients, this makes the procedure feel more comfortable overall.
Another important benefit is that the implanted lens is removable if needed. This flexibility means that adjustments can be made in the future if your vision changes or if your eye health requires it. Knowing that the procedure is not permanently fixed in one way can provide added reassurance. It allows your treatment to adapt alongside your long-term eye health.
Many patients achieve excellent visual clarity with minimal disruption to the eye’s natural anatomy. The lens works in harmony with your eye to improve focus and sharpness without altering key structures. With proper assessment and planning, this approach can deliver stable and satisfying results. Overall, ICL surgery offers a balanced solution that combines precision, flexibility, and high-quality vision correction.
Limitations to Consider
Although ICL surgery offers many benefits, it may not be suitable in every situation. If your autoimmune condition is active or poorly controlled, the risk of complications can be higher. Ongoing inflammation may affect how your eyes respond to the procedure and how well they heal afterwards. For this reason, careful timing is essential when considering surgery.
Chronic inflammation can increase the likelihood of discomfort, slower recovery, or less predictable visual outcomes. This does not mean surgery is unsafe, but it does mean that extra caution is required. Understanding these limitations helps you develop realistic expectations about what the procedure can achieve. Being informed allows you to make decisions with greater confidence.
Your surgeon will assess your overall eye health and the stability of your condition before recommending treatment. They will explain whether it is appropriate to proceed or if it would be better to wait until your condition is more stable. With this personalised guidance, you can choose the safest path forward and ensure the best possible outcome for your vision.
Timing of Surgery
Choosing the right time for your surgery is just as important as the procedure itself. If you have an underlying condition, it’s essential that it is stable and well-controlled before moving forward. Planning your surgery at the right moment helps reduce risks and supports a smoother recovery.
- Waiting for your condition to stabilise: Your surgeon will usually recommend surgery only when your condition is under good control. This helps ensure your body is in the best possible state for healing.
- Avoiding flare-ups: It’s best not to schedule surgery during or immediately after a flare-up. During these periods, inflammation can be higher, which may affect both safety and recovery.
- Supporting better healing: When your condition is stable, your eyes are more likely to heal predictably. This can reduce the risk of complications and improve overall comfort after surgery.
- Coordinating with your medical care: Your eye specialist may work alongside your GP or specialist to decide the safest time for surgery. This team approach ensures all aspects of your health are considered.
By carefully choosing the timing of your procedure, you give yourself the best chance of a safe experience and a successful visual outcome. Taking a little extra time to plan properly can make a meaningful difference to your results.
Post-Surgery Healing Process
Healing after ICL surgery is typically quick and straightforward for most patients. You may notice improvements in your vision within a short time, with only mild discomfort in the early stages. However, if you have an autoimmune condition, your healing process may be slightly slower. This is due to the way your immune system responds and manages inflammation.
Because of this, you may require closer monitoring during your recovery period. Your surgeon will keep a careful eye on how your eyes are healing and whether any additional support is needed. You might be asked to attend more frequent follow-up appointments to ensure everything is progressing as expected. This proactive approach helps identify any concerns early.
Regular follow-ups play an important role in ensuring a smooth recovery. They allow your surgeon to adjust your treatment plan if necessary and provide reassurance as your vision improves. By staying consistent with your aftercare, you can support proper healing and reduce the risk of complications. Over time, most patients achieve stable, clear vision with the right guidance and care.
Managing Inflammation After Surgery
After ICL surgery, some degree of inflammation is normal and usually mild. It is part of your body’s natural healing response as your eyes adjust to the procedure. However, if you have an autoimmune condition, you may experience a slightly stronger or more prolonged inflammatory reaction. Understanding this in advance can help you feel more prepared during recovery.
To manage this, your surgeon will typically prescribe anti-inflammatory eye drops. These medications help reduce swelling, ease discomfort, and support proper healing of the eye. You may also be given specific instructions on how often to use the drops and how long to continue them. Following these directions carefully is essential for controlling inflammation effectively.
Sticking to your treatment plan plays a key role in ensuring a smooth and comfortable recovery. Attending follow-up appointments allows your surgeon to monitor inflammation levels and make adjustments if needed. By staying consistent with your care routine, you can help your eyes heal properly and achieve the best possible visual outcome.
Long-Term Eye Health
ICL surgery can significantly improve how clearly you see, but it does not treat your underlying autoimmune condition. This means you will still need ongoing medical care to manage your condition effectively. Keeping your autoimmune disease under control helps protect your eyes and supports the long-term success of the procedure. Understanding this balance is important for maintaining both your vision and overall health.
Regular eye examinations remain an essential part of your long-term care. These check-ups allow your clinician to monitor your eye health, assess the position of the implanted lens, and detect any early changes. Routine visits provide reassurance and help ensure that any issues are addressed promptly. Staying consistent with these appointments is key to preserving your visual results.
Maintaining your overall health also plays a crucial role in long-term visual stability. Following your treatment plan, eating a balanced diet, and managing inflammation all contribute to healthier eyes. By combining regular monitoring with good lifestyle habits, you can support clear and stable vision for years to come.
Lifestyle Factors
Healthy lifestyle habits can make a meaningful difference to both your immune system and your eye health. Eating a balanced diet, getting enough sleep, and managing stress all help your body function more effectively. These everyday choices support healing and improve how your eyes respond after surgery. Over time, they contribute to more stable and comfortable vision.
These factors can also help reduce the likelihood of autoimmune flare-ups. When your condition is well-managed, your body is better able to maintain a steady healing response. Fewer flare-ups mean less inflammation, which is beneficial for your eyes. This stability is particularly important when recovering from or maintaining the results of surgery.
Taking care of your general health can positively influence your surgical outcomes. Patients who follow healthy routines often experience smoother recovery and more predictable results. Small, consistent habits can have a lasting impact on your vision. By looking after your overall wellbeing, you support the long-term success of your treatment.
Communication Between Specialists
When you’re planning eye surgery alongside a condition like rheumatoid arthritis, coordinated care becomes especially important. Your eye surgeon may work closely with your rheumatologist or another specialist to ensure everything is well managed before moving forward. This teamwork helps create a clearer, safer path towards surgery.
- Sharing your medical history: Your specialists may exchange important details about your condition, medications, and overall health. This helps everyone involved make informed decisions about your treatment.
- Ensuring your condition is well controlled: Your rheumatologist can confirm whether your condition is stable enough for surgery. This reduces the risk of complications during and after the procedure.
- Adjusting medications if needed: In some cases, your treatment plan may be reviewed to support healing. Any changes are carefully managed to avoid affecting your overall health.
- Providing consistent guidance: With both specialists working together, you’ll receive clear and consistent advice at every stage from preparation to recovery.
This collaborative approach not only improves safety and outcomes, but also gives you confidence that every aspect of your health is being carefully considered. Knowing that your care team is working together can make the entire process feel much more reassuring and well supported.
Alternative Options
If ICL surgery isn’t the right fit for you, there are still several effective ways to improve your vision. The most suitable option will depend on your eye health, lifestyle, and any underlying conditions you may have. Your surgeon will guide you through the choices so you can feel confident about what comes next.
- Glasses: Glasses remain one of the safest and simplest ways to correct your vision. They are easy to use, non-invasive, and can be updated as your prescription changes over time.
- Contact lenses: Contact lenses offer a more discreet option and can provide excellent visual clarity. Your specialist may recommend specific types that are suitable for your eyes, especially if you have dryness or sensitivity.
- Other laser vision correction procedures: In some cases, procedures such as LASIK surgery or PRK surgery may be considered. These options reshape the cornea and might be suitable depending on your eye measurements and overall health.
- Lens-based alternatives: If laser procedures aren’t ideal, other lens-based treatments may be explored. These can be tailored to your vision needs and are often considered when multiple factors need to be addressed.
Your surgeon will carefully assess your situation and explain which option is the safest and most effective for you. Even if ICL isn’t suitable, you’ll still have reliable ways to achieve clear, comfortable vision.
Importance of Personalised Care
Every autoimmune condition is unique, which means your care should never follow a one-size-fits-all approach. Your medical history, current symptoms, and overall health all influence how your eyes respond to surgery. Because of this, your surgeon will tailor the treatment plan specifically to your needs. This individualised approach helps ensure that every aspect of your care is carefully considered.
Personalised care plays a key role in minimising potential risks. By assessing your condition in detail, your clinician can identify factors that may affect healing or increase inflammation. Adjustments can then be made to your treatment or timing of surgery to improve safety. This careful planning helps create a more controlled and predictable surgical experience.
It also supports the best possible visual outcome. When your treatment is customised, it aligns more closely with your eye structure and health status. This increases the likelihood of achieving clear, stable vision after surgery. With the right personalised approach, you can feel more confident in both the process and the results.
Choosing an Experienced Surgeon
Experience is especially important when dealing with more complex cases, such as those involving autoimmune conditions. A skilled surgeon understands how to assess potential risks and adapt the procedure to suit your individual needs. Their expertise allows them to anticipate challenges and plan accordingly. This level of insight helps ensure that your treatment is both safe and effective.
Choosing a reputable clinic can give you greater confidence in your care. Established centres often follow strict clinical protocols and use advanced diagnostic technology to evaluate your eyes thoroughly. You are also more likely to receive comprehensive pre- and post-operative support. This environment helps create a smoother and more reassuring treatment journey.
Expertise plays a key role in achieving successful results. An experienced surgeon can make precise decisions during surgery and respond effectively to any unexpected situations. Their knowledge also supports better outcomes during recovery and long-term follow-up. By selecting the right specialist, you improve your chances of a safe procedure and clear, stable vision.
When Surgery Should Be Delayed
If your condition is unstable or you are currently experiencing a flare-up, it may be safer to delay surgery. Active inflammation can increase the risk of complications and affect how well your eyes heal afterwards. Proceeding at the wrong time may lead to less predictable results. Waiting until your condition is under control helps create a safer environment for the procedure.
Allowing your body time to stabilise can significantly reduce potential risks. When inflammation is well-managed, your immune system responds more predictably during healing. This improves both comfort and recovery outcomes after surgery. A short delay can make a meaningful difference to the overall success of the treatment.
Your surgeon will guide you on the safest timing based on your current health status. They may also work closely with your specialist to ensure your condition is properly controlled before proceeding. This collaborative approach helps ensure that you are fully prepared for surgery. With the right timing, you can move forward with greater confidence and safety.
FAQs:
- Can you have ICL surgery if you have rheumatoid arthritis?
Yes, you can have ICL surgery if your rheumatoid arthritis is well-controlled. The most important factor is stability, as this reduces the risk of complications. Your surgeon will assess your overall health and how your condition is managed. If everything is stable, many patients achieve excellent results. - Is autoimmune disease a reason to avoid ICL surgery?
Having an autoimmune condition does not automatically mean you should avoid ICL surgery. Suitability depends on how active or stable your condition is at the time. If your disease is well-managed, the risks are generally low. Your surgeon will guide you based on your individual situation. - How does rheumatoid arthritis affect your eyes during surgery?
Rheumatoid arthritis can affect your eyes by causing dryness or inflammation. These issues may influence comfort during recovery and healing afterwards. Your eye specialist will carefully examine your eye surface before surgery. Managing these symptoms beforehand helps improve outcomes. - Why is disease stability important before ICL surgery?
Disease stability is crucial because active inflammation can interfere with healing. If your condition is stable, your body is more likely to respond well to surgery. It also reduces the chance of complications after the procedure. This is why surgeons often recommend waiting if your condition is not fully controlled. - Can dry eye caused by autoimmune disease affect ICL results?
Dry eye can affect how comfortable your eyes feel after surgery. It may also influence the clarity of your vision during recovery. Although ICL surgery does not directly worsen dry eye, existing symptoms should be treated first. Proper management helps ensure better visual outcomes. - Do autoimmune medications affect ICL surgery?
Some medications used to treat autoimmune diseases can affect your immune response. This may slightly increase the risk of infection or slow healing. Your surgeon will review your medication history carefully before surgery. In some cases, they may coordinate with your doctor to optimise your treatment plan. - Is recovery slower if you have an autoimmune condition?
Recovery is usually still quick, but it can be slightly slower in some cases. This depends on how your immune system responds to healing. You may need closer follow-up appointments to monitor progress. With proper care, most patients recover without significant issues. - What precautions are taken for autoimmune patients during surgery?
Your surgeon will carry out a thorough pre-surgical assessment to check your eye health. They will also evaluate inflammation levels and ensure your condition is stable. In some cases, they may work with your specialist to plan your care. These precautions help reduce risks and improve safety. - Can ICL surgery trigger an autoimmune flare-up?
It is uncommon, but surgery can sometimes affect your immune system. This is why timing is very important when planning the procedure. Surgery is usually scheduled when your condition is stable and well-controlled. Careful planning helps minimise the risk of flare-ups. - What happens if ICL surgery is not suitable for you?
If ICL surgery is not the best option, your surgeon will discuss alternatives with you. These may include glasses, contact lenses, or other vision correction procedures. The aim is always to choose the safest and most effective solution. You will receive personalised advice based on your needs.
Final Thoughts: Making a Confident Decision About ICL Surgery
ICL surgery can be a safe and effective option if you have an autoimmune condition such as rheumatoid arthritis, especially when your condition is stable and well-managed. Careful pre-surgical assessment plays a crucial role in determining suitability, as factors like inflammation, dry eye, and medication use need to be considered. When these elements are properly controlled, the risks are significantly reduced, allowing you to benefit from clear and stable vision.
It’s important to remember that every case is unique, and your treatment plan should be tailored to your specific health needs. Close collaboration between your eye surgeon and your specialist ensures that all aspects of your condition are taken into account. This personalised approach helps improve safety, supports better healing, and gives you reassurance throughout the process. If you’d like to find out whether ICL surgery in London is suitable for you, feel free to contact us at Eye Clinic London to arrange a consultation.
References:
- Del Risco, N.E., Talbot, C.L., Moin, K.A., Manion, G.N., Brown, A.H., Walker, S.M., Zhong, P.S., Zhang, H., Hoopes, P.C. and Moshirfar, M. (2024) ‘Visual outcomes of cataract surgery in patients with previous history of implantable collamer lens’, Journal of Clinical Medicine, 13(15), p. 4292. https://www.mdpi.com/2077-0383/13/15/4292
- Kato, S., Shimizu, K. and Igarashi, A. (2019) ‘Vault changes caused by light-induced pupil constriction and accommodation in eyes with an implantable collamer lens’, Cornea, 38(2), pp. 217-220. https://pubmed.ncbi.nlm.nih.gov/30371566/
- Zaldivar, R., Zaldivar, R., Adamek, P. and Cerviño, A. (2022) ‘Intraoperative adjustment of implantable collamer lens vault by lens rotation aided by intraoperative optical coherence tomography’, Journal of Cataract and Refractive Surgery. https://pubmed.ncbi.nlm.nih.gov/35171140/
- Assaf, J.F., Reinstein, D.Z., Zakka, C., Arbelaez, J.G., Boufadel, P., Choufani, M., Archer, T., Ibrahim, P. and Awwad, S.T. (2023) ‘Deep learning-based estimation of implantable collamer lens vault using optical coherence tomography’, American Journal of Ophthalmology, 253, pp. 29-36. https://www.sciencedirect.com/science/article/pii/S0002939423001861
- García-De la Rosa, G., Peris-Martínez, C., and colleagues (2021) ‘Agreement between optical coherence tomography and Scheimpflug tomography for vault measurement after implantable collamer lens implantation’, Archivos de la Sociedad Española de Oftalmología. https://www.sciencedirect.com/science/article/abs/pii/S0181551221003855

