Flashes and Floaters: When Is It an Emergency?

If you suddenly notice flashes of light or new floaters drifting across your vision, it can feel worrying. You might see tiny specks, threads, or shadowy shapes moving as your eyes shift, or brief flickers of light at the edges of your sight. In many cases, these symptoms are linked to natural changes inside the eye, but sometimes they can point to something more serious.
Flashes and floaters often occur due to changes in the vitreous gel inside your eye. As this gel shifts or becomes more fluid with age, it can pull slightly on the retina, creating these visual effects. This is commonly associated with a process called Posterior Vitreous Detachment, which is usually harmless but still worth monitoring.
However, there are situations where these symptoms may indicate a more urgent condition, such as Retinal Detachment. This happens when the retina begins to separate from the back of the eye and requires immediate treatment. Warning signs include a sudden increase in floaters, persistent flashes, a shadow or curtain over your vision, or a rapid decline in sight.
Understanding the difference between normal and concerning symptoms helps you respond appropriately. While mild, occasional floaters are often not a cause for concern, any sudden or dramatic change should never be ignored. Seeking prompt medical assessment ensures that serious conditions are detected early, giving you the best chance of protecting your vision.
What Are Floaters?
Floaters are small shapes that drift across your field of vision. You might notice them as tiny dots, threads, or cobweb-like shadows that move when your eyes move. They can seem to dart away when you try to focus on them, which can feel a bit frustrating at first. These visual effects come from natural changes inside your eye.
- What causes floaters: Floaters form when tiny clumps or strands develop within the vitreous gel inside your eye. As light enters, these clumps cast shadows onto the retina, which is what you perceive as moving shapes.
- Link to age-related changes: They are commonly associated with Posterior vitreous detachment, where the vitreous slowly shrinks and separates from the retina over time. This is a normal part of ageing.
- When you notice them most: Floaters tend to be more visible against bright or plain backgrounds, such as a clear sky or a white wall. This contrast makes the shadows easier to see.
- When to seek medical advice: In most cases, floaters are harmless. However, if you notice a sudden increase, or if they are accompanied by flashes of light, it could indicate a problem such as retinal detachment and should be checked promptly.
While floaters are usually a normal part of ageing, staying aware of changes in your vision is important. If anything feels different or sudden, it’s always safest to have your eyes examined to rule out more serious conditions.
What Are Flashes of Light?
Flashes are brief bursts of light that appear in your vision. You might describe them as flickers, sparks, or lightning-like streaks, often noticed at the edges of your sight. They can even occur when your eyes are closed, which can make them feel particularly unusual.
These flashes are usually caused by mechanical stimulation of the retina. When the vitreous gel inside your eye shifts or pulls slightly, it can tug on the retina and trigger signals. Your brain interprets these signals as light, even though no external light is entering your eye. This is commonly associated with changes such as Posterior Vitreous Detachment.
You may notice flashes more clearly in darker environments, such as at night or in dim lighting. They often appear in your peripheral vision rather than directly in front of you. Occasional flashes can be a normal part of ageing, but if they become frequent, more intense, or occur alongside a sudden increase in floaters, it is important to seek prompt medical advice.
Why Do Floaters Develop?
Floaters commonly develop as part of the natural ageing process. Over time, the vitreous gel inside your eye becomes more liquid and less uniform. As this happens, tiny clumps or strands can form within the gel, which is what you begin to notice drifting across your vision.
These changes are usually gradual and harmless. Many people experience them as the eye undergoes normal ageing, often linked to processes such as Posterior Vitreous Detachment, where the vitreous slowly separates from the retina. While this can sound concerning, it is very common and does not always lead to complications.
In most cases, floaters do not require treatment. Over time, your brain often adapts and learns to ignore them, making them less noticeable in daily life. However, if you notice a sudden increase in floaters, or if they appear alongside flashes of light or changes in vision, it is important to have your eyes assessed promptly to rule out more serious conditions.
Why Do Flashes Occur?
Flashes occur when the vitreous gel inside your eye shifts or pulls slightly on the retina. This is often part of the natural ageing process, as the vitreous gradually shrinks and changes shape over time.
As the gel moves, it can tug on the retina and stimulate it mechanically. Your brain interprets this stimulation as light, even though there is no actual light entering your eye. This is why you may see brief flickers or streaks, commonly linked to changes such as Posterior Vitreous Detachment.
Occasional flashes can be normal and may not indicate a serious problem. However, if you start noticing flashes more frequently, or if they appear suddenly or alongside new floaters or vision changes, it is important to have your eyes checked promptly. These symptoms can sometimes signal a developing condition that needs urgent attention.
Posterior Vitreous Detachment Explained
Posterior vitreous detachment (PVD) is a common cause of sudden flashes and floaters, especially as you get older. It occurs when the vitreous gel inside your eye naturally shrinks and separates from the retina. Although this can feel alarming, it is usually a normal age-related change rather than a serious problem. The symptoms often appear quickly and can be quite noticeable.
- Sudden increase in floaters: You may see small specks, threads, or cobweb-like shapes drifting across your vision. These floaters can seem more obvious when looking at bright backgrounds.
- Flashes of light: Brief flashes, particularly in your peripheral vision, can occur as the vitreous pulls away from the retina. These may come and go over time.
- Typically a harmless condition: In most cases, PVD does not cause permanent vision loss and settles on its own without treatment.
- Importance of eye examination: Although PVD is usually benign, it can sometimes lead to complications such as retinal tear or retinal detachment. An eye examination ensures that your retina has not been affected.
If you notice new flashes or floaters, it’s important to have your eyes checked promptly. Monitoring your condition helps ensure that any complications are detected early and managed effectively.
When Floaters Are Normal
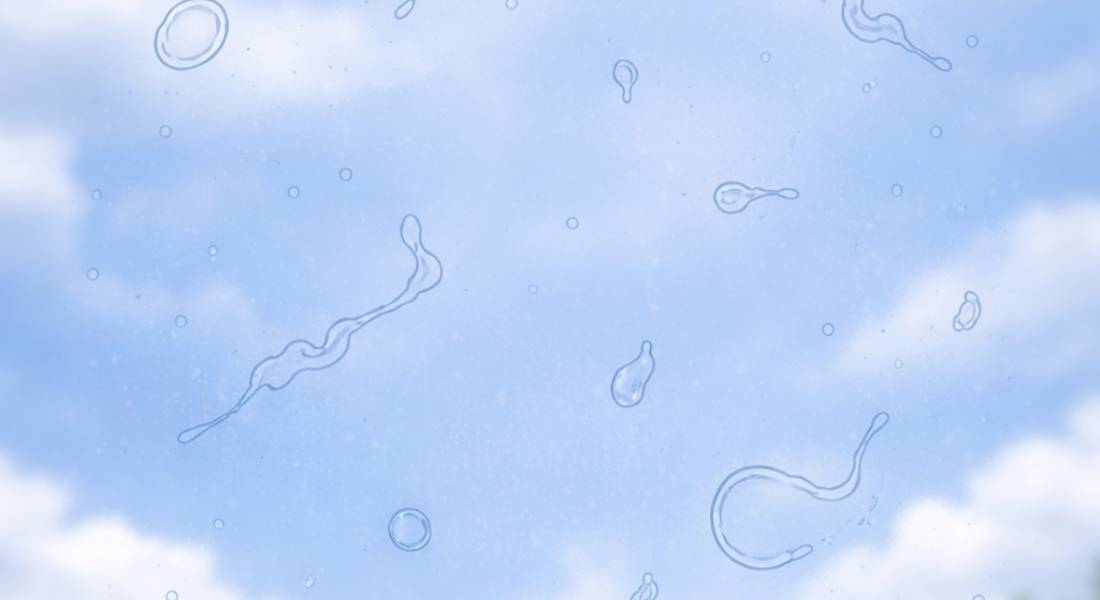
Floaters are usually harmless when they develop gradually. You might notice a few small shapes drifting across your vision, especially against bright backgrounds, but they do not typically interfere with how well you see. These are often part of normal age-related changes inside the eye.
If your floaters remain stable over time and do not suddenly increase, they are less likely to be a cause for concern. Many people find that their brain gradually adapts, making the floaters less noticeable in daily life. This is commonly linked to natural processes such as Posterior Vitreous Detachment, which tends to progress slowly.
Routine eye examinations can help confirm that your floaters are benign. This provides reassurance and ensures there are no underlying issues. When symptoms remain stable, they rarely require any treatment, and simple monitoring is usually all that is needed.
When Flashes Are Not Concerning
Occasional flashes that happen infrequently are often not a cause for concern. You might notice them during normal changes in the vitreous gel, particularly as it shifts with age. These brief flickers can settle on their own without affecting your vision.
If your flashes are short-lived, do not increase in frequency, and are not accompanied by other symptoms, they are less likely to signal a serious problem. This is commonly linked to natural processes such as Posterior Vitreous Detachment. Even so, it is sensible to keep an eye on any changes.
If you are ever unsure, it is always worth seeking professional advice. A simple eye examination can rule out more serious conditions and give you reassurance. Acting early, even for peace of mind, is always a sensible approach when it comes to your vision.
Warning Signs That Require Urgent Attention
When it comes to changes in your vision, some symptoms should never be ignored. While floaters and flashes can often be harmless, a sudden change in their pattern or intensity may signal a more serious underlying issue. Recognising these warning signs early helps you act quickly and protect your sight. Certain symptoms are particularly important to take seriously.
- Sudden increase in floaters or flashes: If you notice a rapid rise in floaters or frequent flashes of light, it may indicate stress or traction on the retina. This can sometimes be linked to conditions such as posterior vitreous detachment or an early retinal tear.
- Shadow or curtain over your vision: A dark shadow, veil, or curtain moving across your field of vision is a key warning sign of retinal detachment. This is a medical emergency that requires immediate attention.
- Blurred vision or sudden vision loss: Any rapid change in clarity, distortion, or loss of vision especially alongside flashes or floaters should be treated as urgent and assessed without delay.
- Need for immediate medical evaluation: These symptoms require prompt examination by an eye specialist or emergency service. Early diagnosis and treatment can prevent permanent damage.
If you experience any of these warning signs, seek medical care straight away. Acting quickly can make a crucial difference in preserving your vision and avoiding long-term complications.
Retinal Tears and Why They Matter
A retinal tear occurs when the delicate surface of your retina is pulled or damaged, often during natural changes in the vitreous gel. As the gel shifts, it can place tension on the retina and create a small break. This is commonly associated with processes such as Posterior Vitreous Detachment.
Once a tear forms, fluid from inside your eye can pass through it and collect underneath the retina. This can cause the retina to lift away from the back of the eye, leading to a more serious condition known as Retinal Detachment. Without treatment, this can result in permanent vision loss.
You may notice warning signs such as a sudden increase in floaters, frequent flashes of light, or new visual disturbances like shadows or blurred areas. These symptoms should never be ignored. Seeking prompt assessment allows the tear to be treated early, often preventing progression and protecting your vision.
Retinal Detachment as an Emergency
Retinal detachment is a serious condition that requires immediate medical attention. It occurs when the retina separates from the back of your eye, disrupting its ability to process light properly. Once this happens, your vision can deteriorate quickly if it is not treated.
You may notice a dark shadow or a curtain-like effect moving across your field of vision. This symptom often worsens over a short period, and parts of your sight may become blocked. These changes are a key warning sign of Retinal Detachment and should never be ignored.
Emergency treatment is needed to reattach the retina and restore its function. Acting quickly significantly improves your chances of preserving vision. Delaying care increases the risk of permanent damage, so if you experience these symptoms, you should seek urgent assessment without hesitation.
Who Is at Higher Risk?
Certain factors can increase your risk of developing retinal problems. These include high myopia (strong short-sightedness), previous eye surgery, or a history of eye injury. As you get older, natural changes in the vitreous gel also make conditions such as Posterior Vitreous Detachment more likely, which can sometimes lead to retinal issues.
If you have a family history of Retinal Detachment, your risk may be higher. Being aware of these factors helps you stay alert to early symptoms such as new floaters, flashes, or changes in your vision. Recognising these signs early allows you to act quickly if needed.
Regular eye examinations are especially important if you fall into a higher-risk group. These checks help detect problems at an early stage, often before symptoms become severe. With consistent monitoring and timely care, you can significantly reduce the risk of complications and protect your long-term vision.
The Role of Eye Trauma
Eye injuries can sometimes trigger sudden flashes and floaters. When your eye experiences an impact or irritation, the internal structures can shift quickly. This may cause the vitreous gel to move abruptly, placing stress on the retina and affecting how you see. The effects of trauma are not always immediate, which is why it’s important to stay alert to changes.
- Sudden vitreous movement: Trauma can disturb the vitreous gel inside your eye, causing it to pull on the retina. This may lead to symptoms such as flashes of light or new floaters.
- Delayed or evolving symptoms: While some symptoms appear straight away, others may develop hours or even days later. Even a minor injury can lead to changes that are not obvious at first.
- Risk to the retina: In some cases, trauma can increase the risk of a retinal tear or retinal detachment. These conditions require prompt diagnosis and treatment to protect your vision.
- Importance of early assessment: After any eye injury, it’s important to have your eye examined, even if symptoms seem mild. Early evaluation helps detect any hidden damage and reduces the risk of complications.
If you experience flashes, floaters, or vision changes after an eye injury, you should seek medical attention promptly. Acting early can prevent further damage and support a better recovery for your vision.
How Doctors Examine Flashes and Floaters
An eye examination is essential to understand what is causing your symptoms. Your doctor will carry out a detailed assessment of the retina using specialised instruments designed to view the back of your eye. This helps identify whether your flashes and floaters are linked to normal changes or something more serious.
Dilating eye drops are usually used to widen your pupils, allowing a clearer and more thorough view of the retina. This makes it easier to detect issues such as small tears or early Retinal Detachment. In some cases, additional imaging tests may be performed to provide more detailed information.
The examination itself is quick and generally painless, although your vision may remain slightly blurred for a short time afterwards due to the drops. Most importantly, it provides valuable insight into your eye health. An accurate diagnosis ensures that, if needed, you receive the right treatment at the right time to protect your vision.
Treatment Options for Floaters
In most cases, floaters are harmless and do not need treatment. Over time, your brain learns to adapt to their presence, and they often become less noticeable. This natural adjustment means that many people find their symptoms improve without any intervention. However, treatment may be considered if floaters significantly affect your vision or daily life.
- Observation and adaptation: For the majority of people, no active treatment is needed. Floaters linked to posterior vitreous detachment tend to settle as your brain gradually ignores them.
- Laser treatment (vitreolysis): In selected cases, laser therapy can be used to break up larger floaters, making them less visible. This option is not suitable for everyone and depends on the size and position of the floaters.
- Surgical treatment (vitrectomy): A vitrectomy involves removing the vitreous gel and replacing it with a clear solution. This can be effective but is usually reserved for severe cases due to potential risks.
- Personalised decision-making: The choice of treatment depends on how much the floaters interfere with your vision. An eye specialist will assess your symptoms and advise whether treatment is appropriate.
Most floaters can be managed without intervention, but if they become disruptive, there are options available. A personalised approach ensures that any treatment balances effectiveness with safety.
Managing Flashes Safely
Flashes themselves are not treated directly. Instead, your doctor focuses on identifying and managing the underlying cause. In many cases, especially when flashes are linked to natural changes such as Posterior Vitreous Detachment, careful monitoring is the first step.
If no retinal damage is found during your examination, you may not need immediate treatment. However, follow-up appointments are important to ensure that your condition remains stable and that no new problems develop. This ongoing observation helps catch any changes early.
You should report any increase in flashes, a sudden rise in floaters, or new visual symptoms straight away. These changes can sometimes indicate a developing issue such as Retinal Detachment. Staying alert to your symptoms and acting quickly if they change is key to protecting your vision.
The Importance of Early Detection

Early detection of retinal problems plays a crucial role in protecting your vision. Treating a small tear is far simpler and more effective than managing a full Retinal Detachment. Acting at the right time can prevent more serious complications and preserve your sight.
Regular eye examinations help identify changes before they become severe. These checks can detect issues linked to natural processes such as Posterior Vitreous Detachment, as well as early signs of retinal damage. Being aware of warning symptoms like new floaters, flashes, or shadows in your vision also helps you take action quickly.
Delaying assessment increases the risk of complications and can reduce treatment success. Prompt medical care gives you the best chance of a positive outcome. By staying proactive and seeking help early, you give yourself the strongest protection for your long-term vision.
How to Monitor Symptoms at Home
It’s important to stay aware of any changes in your vision, especially if you notice floaters or flashes. Paying close attention helps you recognise when something is stable and when it may be changing. This awareness allows you to act quickly if needed. Keeping track of your symptoms can make a real difference.
- Notice patterns in floaters and flashes: Try to observe how many floaters you see and how often flashes occur. Changes in frequency or appearance can provide useful clues about what’s happening inside your eye.
- Watch for sudden increases: If you experience a rapid rise in floaters or new flashes, do not ignore it. These changes can sometimes be linked to conditions such as retinal detachment and require prompt evaluation.
- Keep a simple record: Making a note of when symptoms start, how they change, and any associated effects (like blurred vision) can help you and your doctor understand the pattern more clearly.
- Support early detection and care: Sharing this information with your eye specialist allows for quicker, more accurate assessment. Early detection can prevent complications and protect your vision.
By monitoring your symptoms and acting promptly when changes occur, you take an active role in protecting your eyesight. This simple habit can help ensure that any potential issues are identified and managed early.
Psychological Impact of Visual Disturbances
Flashes and floaters can feel unsettling, especially when they appear suddenly. It is completely natural for you to worry about your vision or fear that something serious may be happening. These thoughts can increase anxiety, particularly if you are unsure about the cause of your symptoms.
Understanding what is behind your symptoms often brings a sense of reassurance. In many cases, flashes and floaters are linked to common, age-related changes such as Posterior Vitreous Detachment, which are usually not harmful. Having clear, accurate information helps reduce uncertainty and makes the situation feel more manageable.
Seeking professional advice can also help you feel more in control. An eye examination can rule out serious conditions like Retinal Detachment and confirm whether monitoring is all that is needed. Knowing when to act and when not to worry gives you confidence and supports your peace of mind, which is just as important as your physical eye health.
FAQs:
- Are flashes and floaters always a sign of an eye emergency?
No, flashes and floaters are often harmless and part of normal ageing. However, a sudden increase in symptoms or associated vision changes can indicate a serious problem. It is important to have new or worsening symptoms checked promptly. Early assessment helps rule out emergencies. - What causes a sudden increase in floaters?
A sudden increase in floaters is often linked to changes in the vitreous gel, such as posterior vitreous detachment. In some cases, it may indicate a retinal tear or bleeding inside the eye. This is why sudden changes should never be ignored. Prompt examination is essential. - When should I seek urgent care for flashes and floaters?
You should seek immediate medical attention if you notice a sudden surge in floaters, frequent flashes, or a shadow in your vision. These symptoms can indicate retinal detachment. Acting quickly can prevent permanent vision loss. Do not delay assessment. - Can floaters go away on their own?
Floaters often become less noticeable over time as your brain adapts to them. In some cases, they may settle below your line of sight. However, they do not always disappear completely. Persistent or worsening floaters should be evaluated. - Are flashes of light dangerous?
Occasional flashes may not be harmful, especially if they occur infrequently. However, repeated or increasing flashes can indicate traction on the retina. This may lead to a tear or detachment. It is important to monitor any changes. - What is posterior vitreous detachment (PVD)?
Posterior vitreous detachment is a common age-related condition where the vitreous gel separates from the retina. It often causes flashes and floaters. While usually harmless, it can sometimes lead to retinal tears. An eye examination is recommended to confirm safety. - Can stress or fatigue cause flashes or floaters?
Stress and fatigue do not directly cause floaters, but they may make you more aware of visual disturbances. Migraines triggered by stress can cause flashing lights or visual patterns. It is important to distinguish these from retinal symptoms. Medical advice can help clarify the cause. - Who is most at risk of retinal detachment?
People with high myopia, previous eye surgery, eye injuries, or a family history of retinal detachment are at higher risk. Ageing also increases the likelihood. Being aware of these risk factors helps with early detection. Regular eye checks are important. - How are flashes and floaters diagnosed?
An eye specialist will perform a detailed examination of the retina using dilating drops and specialised equipment. Imaging tests may also be used. This helps detect tears, detachment, or other issues. The process is usually quick and painless. - Can flashes and floaters be prevented?
While age-related changes cannot be prevented, you can reduce risk by protecting your eyes from injury and attending regular eye examinations. Managing conditions like diabetes and high myopia also helps. Early detection is the most effective way to prevent complications.
Final Thought: Acting Early Can Protect Your Vision
Flashes and floaters are common visual experiences, but understanding when they signal something more serious is essential. While many cases are harmless and related to natural ageing, sudden changes in symptoms should never be ignored. Recognising warning signs such as a rapid increase in floaters, frequent flashes, or a shadow in your vision can make a crucial difference in preserving your sight.
Early assessment allows eye specialists to detect retinal tears or detachment before they progress. Timely treatment can prevent long-term damage and significantly improve outcomes. Staying aware of your symptoms and seeking prompt care when needed is the best way to protect your vision.
If you are experiencing persistent or concerning symptoms, professional guidance is important. If you’re considering floaters treatment in London and want to know if it’s the right option, you’re welcome to reach out to us at Eye Clinic London to book a consultation.
References:
- Shah, C.P. and Heier, J.S. (2017), YAG laser vitreolysis vs sham YAG vitreolysis for symptomatic vitreous floaters: a randomized clinical trial, JAMA Ophthalmology, 135(9), pp. 918–923. https://jamanetwork.com/journals/jamaophthalmology/fullarticle/2643488
- Wroblewska-Czajka, E. et al. (2023), Laser vitreolysis in patients with symptomatic vitreous floaters, International Journal of Environmental Research and Public Health, 20(1), pp. 1–10. https://pubmed.ncbi.nlm.nih.gov/36543595/
- Katsanos, A., Tsaldari, N., Gorgoli, K., Lalos, F., Stefaniotou, M. and Asproudis, I. (2020), Safety and efficacy of YAG laser vitreolysis for the treatment of vitreous floaters: an overview, Advances in Therapy, 37(4), pp. 1319–1327. https://pubmed.ncbi.nlm.nih.gov/32086749/
- Murakami, K., Jalkh, A.E., Avila, M.P., Trempe, C.L. and Schepens, C.L. (1983) Vitreous floaters, Ophthalmology, 90(11), pp. 1271–1276. https://www.sciencedirect.com/science/article/pii/S016164208334392X
- Wang, Y., Zhao, X. and Liu, J. (2019) Imaging vitreous floaters and cataracts with optical simulations, Optik, 194, 163075. https://www.sciencedirect.com/science/article/pii/S0030402619309660

