Can Neuropathic Eye Pain Be Chronic? Long-Term Outlook Explained

Neuropathic eye pain can feel confusing and frustrating, especially when your symptoms continue even though the eye appears normal during examination. If you experience ongoing discomfort that does not improve with common eye treatments, nerve-related pain may be the underlying cause. Modern ophthalmology now recognises neuropathic eye pain as a genuine condition that can sometimes become chronic. Understanding this can help explain why symptoms may persist.
Unlike irritation caused by dryness or infection, neuropathic eye pain originates from abnormal nerve signalling. The nerves responsible for sensing the surface of your eye may become hypersensitive. When this happens, they can continue sending persistent pain signals to the brain even when the surface appears healthy. This process can lead to long-lasting discomfort without visible injury.
Understanding the long-term outlook is important because early diagnosis can improve symptom control. When nerve sensitivity is identified and managed appropriately, many patients experience gradual improvement. Treatment often focuses on calming nerve activity and protecting the ocular surface. Ongoing research is also helping doctors better understand how chronic neuropathic pain develops and how it can be managed more effectively.
Understanding Neuropathic Eye Pain
Neuropathic eye pain occurs when the sensory nerves in your eye become damaged or overly sensitive. These nerves normally help detect irritation and protect the eye from injury. When their signalling becomes abnormal, they may begin sending pain signals even without visible disease. This can lead to persistent discomfort despite a healthy-appearing eye surface.
You may experience sensations such as burning, stabbing, aching, or electric-like pain. Many people also notice increased sensitivity to light, wind, or touch around the eyes. These symptoms can feel intense and may occur even when routine examinations appear normal. This mismatch between symptoms and clinical findings is a common feature of neuropathic eye pain.
Because the condition involves changes in nerve signalling rather than obvious structural damage, diagnosis can sometimes take time. Your doctor will usually evaluate your symptoms carefully and rule out other eye conditions first. Additional tests may also be used to assess nerve function and ocular surface health. Once neuropathic pain is identified, treatment can be tailored to your specific needs.
Why Neuropathic Eye Pain Can Become Chronic
Neuropathic eye pain can become chronic when the nerve pathways responsible for sensation remain sensitised over time. Repeated irritation, inflammation, or injury may cause these nerves to send exaggerated signals to the brain. This process is known as nerve hypersensitivity. When it develops, the nerves no longer respond only to genuine irritation.
As hypersensitivity increases, your nervous system may become more reactive to everyday stimuli. Simple factors such as wind, blinking, or normal light exposure may begin to trigger discomfort. These sensations can feel much stronger than expected. Over time, the nervous system may continue reinforcing this heightened response.
Chronic symptoms occur when nerve signalling does not return to normal after the original trigger has resolved. Even when the eye surface appears healthy, the nerves may continue producing pain signals. This is why early recognition and treatment are important. Addressing nerve-related pain promptly can reduce the risk of long-term complications.
The Importance of Corneal Nerves
Your cornea contains one of the highest concentrations of sensory nerves in the body. These nerves help detect irritation and play an important role in maintaining healthy tear production. They also trigger protective reflexes such as blinking. Together, these responses help keep your eyes safe and comfortable.
When these nerves become damaged or disrupted, the signals they send may change. Even minor environmental triggers such as wind or light may cause significant discomfort. You might experience sensations that feel far more intense than expected. This is why symptoms can sometimes seem disproportionate to what doctors observe during examination.
Modern imaging techniques now allow clinicians to study corneal nerves in much greater detail. One example is corneal confocal microscopy, which can visualise microscopic nerve structures. This technology helps doctors detect subtle nerve damage that may not be visible during routine exams. As a result, it has greatly improved the understanding and diagnosis of neuropathic eye pain.
Common Causes of Neuropathic Eye Pain

Neuropathic eye pain can sometimes develop after long-term dry eye disease. When dryness persists, inflammation on the eye surface may irritate and damage corneal nerve fibres. Over time, this irritation can disrupt how sensory signals are transmitted. As a result, the nerves may become overly sensitive.
Eye surgery can also influence nerve sensitivity in certain cases. Procedures such as LASIK or cataract surgery temporarily disturb the corneal nerves while the eye heals. Most patients recover without complications as the nerves regenerate. However, in a small number of people, nerve irritation may persist and lead to ongoing discomfort.
Other possible causes include eye infections, trauma, autoimmune conditions, and prolonged ocular inflammation. These factors can interfere with the normal function of sensory nerves in the cornea. When nerve pathways remain unstable, pain signals may continue even after the original problem improves. This ongoing signalling can contribute to chronic neuropathic eye pain.
Symptoms That Suggest Neuropathic Pain
Symptoms of neuropathic eye pain often feel different from the irritation you might experience with common eye conditions. The discomfort may seem unusual because it is related to nerve signalling rather than surface inflammation. As a result, symptoms can appear even when the eye looks relatively normal during examination.
- Burning, stinging, or shooting sensations: People with neuropathic eye pain frequently describe sharp or burning discomfort. The sensation may feel persistent or occur in sudden bursts. These feelings are often stronger than typical dryness-related irritation.
- Pain without obvious eye redness or damage: One notable feature is that symptoms may appear severe even when the eye surface looks healthy. This mismatch between symptoms and clinical findings can be an important clue for clinicians.
- Significant light sensitivity: Bright light, sunlight, or computer screens may quickly trigger discomfort. You might find yourself avoiding well-lit environments because the sensitivity becomes difficult to tolerate.
- Limited relief from standard dry eye treatments: Artificial tears and other lubricating treatments may provide only mild or temporary improvement. Because the underlying problem involves nerve signalling rather than tear deficiency, these treatments often fail to resolve the pain completely.
Recognising these patterns can help clinicians identify neuropathic involvement. When symptoms do not match typical dry eye findings, further evaluation may be needed to determine whether nerve hypersensitivity is contributing to the discomfort.
Differences Between Dry Eye and Neuropathic Pain
Dry eye disease and neuropathic eye pain can sometimes occur together, which may make diagnosis more difficult. Dry eye typically develops when your tear film becomes unstable or when inflammation affects the ocular surface. Neuropathic pain, however, is primarily related to abnormal nerve signalling. The discomfort originates from nerve hypersensitivity rather than tear deficiency alone.
If you have neuropathic eye pain, you may report severe discomfort even when examination findings appear minimal. In contrast, dry eye disease often presents with visible signs such as redness, tear film instability, or surface irritation. This difference between symptoms and clinical findings can help doctors distinguish between the two conditions. Recognising these patterns helps guide appropriate treatment.
In some cases, both conditions exist at the same time. Chronic dry eye may irritate corneal nerves and gradually lead to nerve hypersensitivity. Over time, this irritation can evolve into neuropathic pain. Addressing both tear film problems and nerve sensitivity usually leads to better symptom control.
The Role of Nerve Sensitisation
Nerve sensitisation occurs when sensory nerves become unusually responsive to stimulation. This change can develop after injury, inflammation, or repeated irritation of the eye. Once sensitisation develops, the nervous system may begin amplifying pain signals.
In neuropathic eye pain, this means that mild triggers can produce strong discomfort. Normal activities such as blinking, exposure to light, or wind may suddenly feel painful. The brain essentially becomes more alert to signals coming from the eye.
- Increased sensitivity to normal stimuli: Sensitised nerves react more strongly than usual. Everyday sensations that would normally be harmless may trigger pain or irritation.
- Amplified pain signals: The nervous system can magnify signals travelling from the eye to the brain. As a result, discomfort may feel far more intense than the physical condition of the eye would suggest.
- Persistent symptoms after healing: Even when the original injury or inflammation improves, nerve pathways may remain overly sensitive. This can cause ongoing discomfort despite a healthy-looking eye surface.
Reducing nerve sensitisation often requires specialised treatment strategies. Doctors may focus on calming nerve activity while also protecting the ocular surface from additional irritation. Over time, this approach may help restore more balanced nerve responses and improve overall comfort.
Central Sensitisation and Brain Involvement
Neuropathic eye pain does not occur only within the eye itself. Your brain also plays a major role in how pain signals are interpreted. When nerve signals from the eye are repeatedly activated, the brain may become more sensitive to them. This increased responsiveness can intensify how discomfort is perceived.
This process is known as central sensitisation. It means the nervous system becomes more efficient at detecting and amplifying pain signals. As a result, even mild stimuli such as light, wind, or blinking may feel unusually painful. The heightened response occurs because the brain processes these signals differently.
Understanding this mechanism helps explain why symptoms may persist over time. In some cases, treatment must address both the eye surface and the nervous system. Therapies may focus on calming nerve activity and improving pain regulation. Managing the entire pain pathway often leads to better symptom control.
How Doctors Diagnose Neuropathic Eye Pain
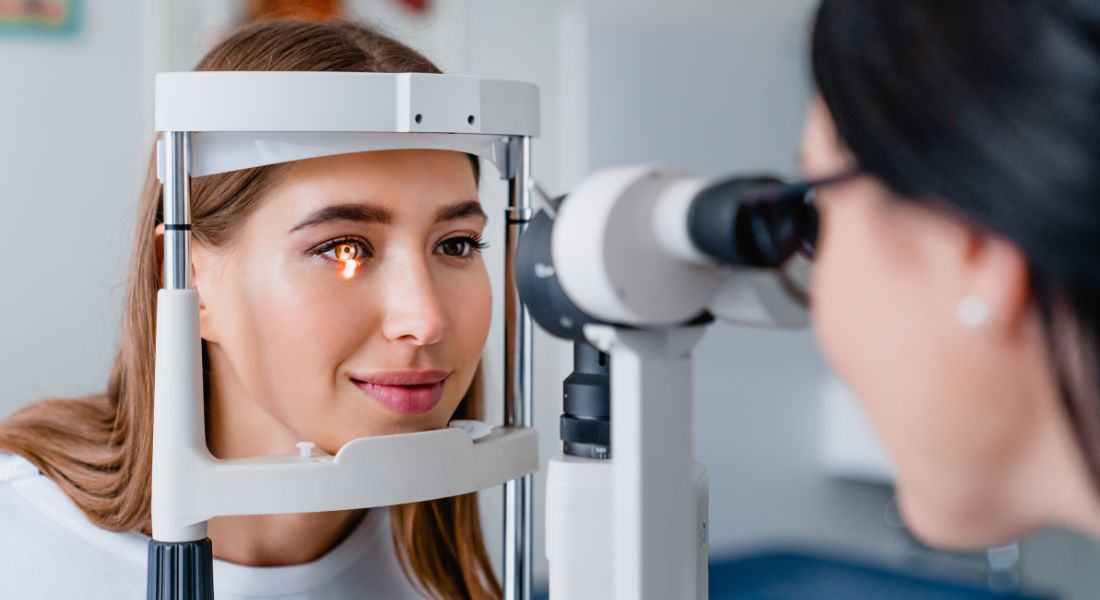
Diagnosing neuropathic eye pain usually begins with a detailed clinical history. Your doctor will ask about your symptoms, when they started, and what factors seem to trigger or worsen them. Previous eye conditions, injuries, or surgeries may also be discussed. This information helps identify whether nerve involvement might be contributing to your discomfort.
A comprehensive eye examination is then performed to rule out more common causes such as infection, inflammation, or severe dry eye. If your symptoms appear much more intense than the clinical findings suggest, neuropathic pain may be considered. Doctors may also evaluate how your symptoms respond to standard treatments. These observations provide important diagnostic clues.
In some cases, specialised imaging techniques are used to study the corneal nerves in greater detail. One example is confocal microscopy, which allows clinicians to view microscopic nerve fibres within the cornea. This technology can reveal subtle nerve abnormalities that are not visible during routine examinations. As a result, it has significantly improved the accuracy of diagnosing neuropathic eye pain.
The Long-Term Outlook for Neuropathic Eye Pain
The long-term outlook for neuropathic eye pain can vary from person to person. Much depends on the underlying cause, the extent of nerve involvement, and how early the condition is recognised. Some patients notice gradual improvement as nerve activity stabilises over time.
In other cases, symptoms may persist for longer and require ongoing management. Nerve tissue heals slowly, so progress can sometimes take months rather than weeks. Consistent treatment and follow-up care are often important for maintaining stability.
- Gradual improvement is possible: In many individuals, nerve sensitivity decreases as the healing process continues. As nerve signalling becomes more balanced, discomfort may gradually reduce.
- Some patients require long-term management: When nerve hypersensitivity persists, treatment may focus on controlling symptoms rather than completely eliminating them. Regular monitoring helps ensure therapies remain effective.
- Earlier diagnosis improves outcomes: When neuropathic eye pain is recognised early, targeted treatments can begin sooner. This may reduce the risk of symptoms becoming chronic.
- Advances in treatment are improving care: Ongoing research continues to expand understanding of nerve-related eye pain. New diagnostic methods and therapies are helping clinicians manage the condition more effectively.
With appropriate care, many patients experience meaningful relief and improved daily comfort. Even when symptoms do not disappear completely, a well-planned treatment strategy can significantly improve quality of life.
Importance of Early Diagnosis
Early diagnosis is one of the most important factors in preventing chronic neuropathic eye pain. When nerve irritation is recognised and treated quickly, hypersensitivity may not become permanent. Addressing the problem early allows doctors to stabilise nerve signalling before symptoms worsen. This often leads to better long-term outcomes.
If diagnosis is delayed, the nerve pathways may become increasingly reactive. You might spend months treating dry eye symptoms before the nerve-related cause is identified. During this time, the nervous system can continue reinforcing the pain response. This delay may allow symptoms to persist for longer than necessary.
Specialist evaluation can help identify nerve-related pain at an earlier stage. Once neuropathic mechanisms are recognised, treatment can focus on calming nerve activity and protecting the ocular surface. This targeted approach improves the chances of symptom control. Early recognition plays a key role in reducing the risk of chronic discomfort.
Tear Film Support in Treatment
Supporting your tear film remains an important part of managing neuropathic eye pain. A stable tear layer helps protect the corneal nerves from environmental irritation. When the eye surface stays well lubricated, it reduces stress on sensitive nerve endings. Lubricating drops can help maintain this protective barrier.
Artificial tears and protective gels are often recommended as part of treatment. These products reduce friction that occurs during blinking and help keep the eye surface hydrated. Regular use may improve overall comfort and reduce surface irritation. Maintaining moisture also helps stabilise the ocular environment.
Although tear support alone may not completely eliminate neuropathic pain, it can reduce triggers that worsen symptoms. A healthier ocular surface allows the nerves more opportunity to recover. This supportive care works alongside other treatments that target nerve activity. Together, these approaches help improve long-term symptom control.
Anti-Inflammatory Treatment
Inflammation can play an important role in nerve irritation within the eye. When inflammatory processes are active, they may sensitise the delicate nerve endings in the cornea. Reducing this inflammation helps create a more stable environment for the nerves and can improve overall symptom control.
Doctors may recommend medications that calm immune activity within the eye. These treatments work by lowering the levels of inflammatory chemicals that can irritate nerve fibres. As inflammation decreases, nerve sensitivity may gradually improve.
- Reducing inflammation protects corneal nerves: Controlling inflammatory activity helps prevent additional irritation to already sensitive nerve endings. This creates a healthier environment for healing.
- Medications may regulate immune responses: Certain treatments are designed to reduce inflammatory signalling in the eye. By calming these responses, irritation and discomfort may become less intense.
- Lower inflammation can reduce pain intensity: When inflammatory chemicals decrease, nerve endings often become less reactive. This can help reduce burning or stinging sensations.
- Combination therapy often works best: Anti-inflammatory treatments are usually used alongside other therapies that address nerve signalling and ocular surface protection. Treating multiple factors at the same time often improves outcomes.
A comprehensive treatment plan that targets both inflammation and nerve sensitivity is often essential for managing neuropathic eye pain effectively. Regular monitoring allows clinicians to adjust therapy and maintain long-term symptom control.
Neuromodulating Medications

Neuromodulating medications help regulate abnormal nerve activity that contributes to neuropathic eye pain. These medicines are commonly used to treat other types of nerve-related pain. They work by reducing the intensity of signals that nerves send to the brain. By calming this activity, they may help decrease persistent discomfort.
You may notice improvement gradually rather than immediately. Over time, the intensity and frequency of pain can begin to decrease. Doctors usually start with a carefully controlled dose and adjust it if needed. Regular monitoring helps ensure the treatment remains safe and effective.
These medications are typically considered when symptoms remain persistent despite other therapies. They form part of a broader strategy that focuses on reducing nerve hypersensitivity. Treatment is usually guided by a specialist familiar with neuropathic pain. Careful supervision helps achieve the best possible outcomes.
Lifestyle Adjustments That Help
Certain lifestyle adjustments can help reduce triggers that worsen neuropathic eye pain. You may notice that factors such as prolonged screen time, harsh lighting, or dry environments increase discomfort. Making small changes to these conditions can improve daily comfort. These practical steps help reduce unnecessary stress on sensitive eyes.
Taking regular breaks from digital devices allows your eyes to rest and recover. You can also improve comfort by maintaining good indoor humidity, which helps prevent excessive tear evaporation. Avoiding direct airflow from fans, air conditioners, or vents can further reduce irritation. These simple adjustments often make a noticeable difference.
Lifestyle changes are designed to support medical treatment rather than replace it. By reducing environmental triggers, you give sensitive nerves a better chance to stabilise. Over time, these habits can help maintain a more comfortable eye environment. Consistency in your daily routine plays an important role in managing symptoms.
Emotional Impact of Chronic Eye Pain
Chronic eye pain can affect more than just physical comfort. When discomfort continues for a long time, it may begin to influence your emotional wellbeing and daily routine. Activities such as working on a computer, reading, or driving may become more difficult, which can lead to frustration or anxiety.
- Daily activities may become challenging: Persistent eye discomfort can make routine tasks harder to manage. Concentration, screen use, and exposure to bright environments may all feel more uncomfortable.
- Unclear symptoms can create confusion: Some patients feel uncertain when symptoms continue even though eye examinations appear normal. This mismatch between symptoms and visible signs can be difficult to understand.
- Understanding the neurological basis can provide reassurance: Learning that neuropathic eye pain originates from nerve signalling rather than visible damage can help explain the symptoms. It confirms that the discomfort is real, even when clinical findings are limited.
- Support from experienced clinicians is important: Clear explanations and structured treatment plans often help restore confidence. Knowing what is happening and how it can be managed makes the condition easier to cope with.
Addressing emotional wellbeing is an important part of long-term care. With the right support and guidance, you can better manage symptoms and regain a sense of control over your daily life.
Research Advancements in Neuropathic Eye Pain
Scientific understanding of neuropathic eye pain has advanced significantly in recent years. Researchers are now exploring how corneal nerves respond to injury and how they regenerate during the healing process. These insights are helping clinicians develop more effective treatment strategies.
- Growing research on corneal nerve regeneration: Scientists are studying how corneal nerves repair themselves after injury or surgery. Understanding this process helps doctors recognise why some patients recover normally while others develop persistent nerve sensitivity.
- Improved diagnostic technologies: Modern imaging techniques now allow clinicians to examine microscopic nerve structures in the cornea with greater clarity. These tools help identify nerve abnormalities that were previously difficult to detect.
- Earlier diagnosis and intervention: With better diagnostic methods, doctors can identify neuropathic changes sooner. Early recognition allows treatment to begin earlier, which may improve long-term outcomes.
- Development of targeted medications: Researchers are also investigating medications that specifically influence nerve signalling pathways. These therapies aim to stabilise hypersensitive nerves and reduce abnormal pain signals.
Ongoing research continues to expand knowledge about neuropathic eye pain. As new discoveries emerge, clinicians are gaining more tools to diagnose the condition accurately and manage symptoms more effectively in the future.
When Symptoms Persist Long Term
Some people experience neuropathic eye pain for extended periods. If nerve hypersensitivity continues, you may need ongoing treatment and monitoring. Although symptoms can persist, long-term management often helps reduce discomfort. Many patients notice gradual improvement with consistent care.
Regular follow-up appointments allow your doctor to review your progress and adjust treatment if needed. As nerve function changes over time, therapies may be modified to maintain symptom control. Monitoring helps ensure that your treatment plan remains effective. This approach supports long-term stability.
You may also develop personal strategies that help manage triggers more effectively. Combining medical treatment with practical lifestyle adjustments can improve daily comfort. Over time, these steps help you maintain better control of symptoms. With proper management, the long-term outlook often becomes more positive.
Future Therapies Under Investigation
Researchers are actively exploring new ways to treat neuropathic eye pain, particularly therapies that address nerve hypersensitivity more precisely. As scientific understanding of corneal nerves improves, treatment strategies are becoming more targeted and sophisticated.
- Medications designed for ocular nerve pain: New drug therapies are being studied that specifically target the nerve pathways responsible for pain signalling in the eye. These treatments aim to reduce abnormal nerve activity without affecting normal eye function.
- Regenerative therapies for nerve repair: Scientists are investigating methods to encourage healthy nerve regeneration within the cornea. By supporting proper nerve repair, these therapies may help restore normal sensation and reduce persistent discomfort.
- Improved treatment precision: Advances in research are helping doctors better understand how nerve signalling works in the eye. This knowledge allows therapies to be tailored more accurately to the underlying cause of symptoms.
- Expanding options for personalised care: As new treatments are developed, clinicians may be able to choose therapies that match each patient’s specific condition and nerve response patterns.
Ongoing research continues to shape the future of neuropathic eye pain management. With better understanding of nerve biology and pain pathways, future therapies are expected to provide more effective and personalised care for patients experiencing persistent eye discomfort.
Why Specialist Care Is Important
Neuropathic eye pain often requires specialised evaluation. Experienced clinicians understand how nerve hypersensitivity affects sensation in the eyes. Their expertise helps them recognise patterns that may not be obvious during a routine examination. This knowledge improves both diagnosis and treatment planning.
A specialist can identify when nerve-related pain is likely to be contributing to your symptoms. They may recommend treatments that are not typically used for routine eye irritation or dry eye disease. These therapies focus on calming nerve activity and protecting the ocular surface. A targeted approach often leads to better symptom control.
Seeking specialist care also ensures that your treatment addresses the underlying cause of discomfort. Early intervention may help prevent nerve hypersensitivity from becoming more severe. Clear guidance from an experienced clinician can make the treatment process easier to understand. With expert support, many patients achieve better long-term outcomes.
FAQs:
- Can neuropathic eye pain last for years?
Yes, neuropathic eye pain can persist for a long time in some individuals. Because the condition involves abnormal nerve signalling rather than visible surface damage, symptoms may continue even after the original cause has resolved. With appropriate diagnosis and long-term management, many people experience gradual improvement in their symptoms over time. - Is neuropathic eye pain permanent?
Neuropathic eye pain is not always permanent. In many cases, nerve sensitivity decreases gradually as the nervous system stabilises. Recovery may take time because nerve tissue heals slowly, but consistent treatment and supportive care can significantly reduce symptoms for many patients. - Why does neuropathic eye pain occur even when the eye looks normal?
This condition affects the nerves responsible for sensing the eye rather than the visible structures themselves. When these nerves become hypersensitive, they can continue sending pain signals even when the surface of the eye appears healthy. This is why symptoms may feel severe despite minimal findings during an examination. - How is neuropathic eye pain different from dry eye disease?
Dry eye disease is primarily related to tear film instability and inflammation on the eye surface. Neuropathic eye pain, however, develops when the nerves that detect sensation become overly sensitive or dysfunctional. Although the two conditions can occur together, neuropathic pain is driven mainly by abnormal nerve signalling rather than tear deficiency alone. - Can dry eye disease lead to neuropathic eye pain?
Yes, long-term dry eye disease can sometimes contribute to neuropathic eye pain. Persistent dryness and inflammation may irritate the corneal nerves and disrupt normal nerve signalling. Over time, this irritation can cause the nerves to become hypersensitive, leading to ongoing discomfort. - What treatments are available for chronic neuropathic eye pain?
Treatment usually focuses on reducing nerve hypersensitivity while protecting the eye surface. Doctors may recommend lubricating eye drops, anti-inflammatory medications, or neuromodulating therapies that calm abnormal nerve activity. The exact treatment plan depends on the underlying cause and severity of symptoms. - How long does it take for neuropathic eye pain to improve?
Improvement can vary from person to person. Some individuals notice relief within several months once treatment begins, while others may require longer periods of management. Because nerve recovery occurs slowly, gradual progress is common rather than immediate resolution. - Can lifestyle changes help manage neuropathic eye pain?
Lifestyle adjustments can support medical treatment and reduce symptom triggers. Reducing screen time, maintaining good indoor humidity, and avoiding direct airflow from fans or air conditioners can help minimise irritation. These steps create a more comfortable environment for sensitive eyes. - Is neuropathic eye pain difficult to diagnose?
Neuropathic eye pain can sometimes be challenging to diagnose because the eye may appear normal during examination. Doctors typically rule out other common causes of eye discomfort before considering nerve involvement. Specialised imaging techniques and careful evaluation of symptoms can help confirm the diagnosis. - When should you see a specialist for persistent eye pain?
You should consider seeing a specialist if eye discomfort continues despite treatment for common conditions such as dry eye or irritation. Persistent pain, especially when examination findings appear minimal, may suggest nerve involvement. A specialist can evaluate your symptoms more thoroughly and recommend targeted treatments.
Final Thought: Moving Forward with Neuropathic Eye Pain Treatment
Neuropathic eye pain can feel confusing, especially when your symptoms persist even though your eyes appear normal during examination. Because the condition involves abnormal nerve signalling rather than visible surface damage, it can sometimes take time to identify the true cause of discomfort. Understanding how nerve hypersensitivity develops is an important step toward finding the right approach to care.
Although neuropathic eye pain can become chronic in some cases, many people experience gradual improvement once the condition is properly recognised and managed. Treatment usually focuses on calming nerve activity, protecting the ocular surface, and reducing triggers that worsen symptoms. Early diagnosis often plays a significant role in improving long-term outcomes. If you’re considering neuropathic eye pain treatment and want to know if it’s the right option, you’re welcome to reach out to us at Eye Clinic London to book a consultation.
Reference:
- Galor, A., Levitt, R.C., Felix, E.R., Martin, E.R. and Sarantopoulos, C.D. (2015) ‘Neuropathic ocular pain: an important yet underevaluated feature of dry eye’, Eye, 29(3), pp. 301–312. https://pubmed.ncbi.nlm.nih.gov/22330055/
- Rosenthal, P. and Borsook, D. (2016) ‘Ocular neuropathic pain’, British Journal of Ophthalmology, 100(1), pp. 128–134. https://pubmed.ncbi.nlm.nih.gov/25943558/
- Belmonte, C., Nichols, J.J., Cox, S.M., Begley, C.G., Bereiter, D.A., Gallar, J., Rocha, G.B., Jones, D.B., Nelson, J.D., and others (2017) ‘TFOS DEWS II Pain and Sensation Report’, in TFOS DEWS II, The Ocular Surface Society. https://www.ncbi.nlm.nih.gov/books/NBK542282/
- Valencia‑Sandonís, C., Vázquez, A., Valencia‑Nieto, L., Martínez‑Plaza, E., Blanco‑Vázquez, M., Sobas, E.M., Calonge, M., Ortega, E., Enríquez‑de‑Salamanca, A. and González‑García, M.J. (2025) ‘Long‑Term Evolution of Chronic Neuropathic Ocular Pain and Dry Eye Following Corneal Refractive Surgery’, Journal of Clinical Medicine, 14(13), 4406. https://www.mdpi.com/2077-0383/14/13/4406
- ‘Ocular neuropathic pain in a real‑world patient cohort with dry eye disease: A SAVE Sight Dry Eye Registry study’, Ocular Neuropathic Pain, S2950‑2535(24)00068‑6. Available at: https://www.sciencedirect.com/science/article/pii/S2950253524000686

