What Is Ocular Hypertension? Does It Always Lead to Glaucoma? (Guide)

Hearing that your eye pressure is higher than normal can feel alarming. I still remember a patient asking me, “Does this mean I’ll get glaucoma?” It’s a common concern, and it’s understandable to feel anxious when faced with this diagnosis. Knowing what ocular hypertension really means can help put your mind at ease.
Ocular hypertension refers to consistently elevated intraocular pressure, which is the fluid pressure inside your eyes. While higher pressure can increase the risk of optic nerve damage, it does not automatically mean glaucoma will develop. Many people with ocular hypertension maintain normal vision throughout their lives without any nerve damage.
The key difference between ocular hypertension and glaucoma is that glaucoma involves actual damage to the optic nerve, often accompanied by changes in peripheral vision. Ocular hypertension is a warning sign rather than a disease itself. Regular monitoring allows eye specialists to detect any early changes and intervene promptly if necessary.
Managing ocular hypertension usually involves routine eye examinations, monitoring eye pressure, and sometimes lifestyle adjustments or medications to lower pressure. With proper care and follow-up, most people can protect their vision and reduce the risk of glaucoma, making early awareness and vigilance the most important steps.
Understanding Ocular Hypertension
Ocular hypertension is a condition in which the pressure inside your eyes, called intraocular pressure (IOP), is higher than normal, yet there is no detectable damage to the optic nerve or loss of vision. Essentially, your eyes are under increased pressure, but at this stage, there are no signs of glaucoma. This distinction is important because raised eye pressure alone does not mean you have the disease.
The normal range for IOP is typically between 10 and 21 mmHg. When measurements consistently exceed this range, an eye specialist may diagnose ocular hypertension. It’s crucial to understand that many people with elevated IOP never develop optic nerve damage or glaucoma, and the condition can remain stable for years without affecting vision.
Living with ocular hypertension does mean a slightly higher risk of developing glaucoma over time, which is why regular monitoring is essential. Your eye doctor may recommend periodic pressure checks, visual field tests, and optic nerve imaging to detect any early changes. With careful observation and timely intervention if needed, most people can maintain healthy vision.
How Eye Pressure Is Measured
Measuring intraocular pressure (IOP) is a simple yet highly important part of a comprehensive eye examination. It helps detect conditions such as ocular hypertension and glaucoma before significant vision damage occurs. The procedure is generally quick, minimally uncomfortable, and performed routinely during eye check-ups. Several reliable techniques are used depending on the patient’s needs and clinical situation.
- Goldmann Applanation Tonometry: This method is considered the gold standard for measuring eye pressure due to its accuracy and consistency. A specialized device gently flattens a small area of the cornea to determine the force required, which directly reflects intraocular pressure. It is commonly performed using a slit lamp microscope and provides highly reliable results.
- Non-contact “Air Puff” Tonometry: This quick and painless method uses a controlled puff of air to flatten the cornea momentarily. It does not require direct contact with the eye, making it comfortable and ideal for routine screenings. While slightly less precise than applanation tonometry, it is widely used in general practice settings.
- Rebound or Dynamic Contour Tonometry: These techniques are often used for patients who may not tolerate traditional methods well. Rebound tonometry uses a small probe that briefly touches the cornea without requiring numbing drops. Dynamic contour tonometry measures pressure with minimal influence from corneal thickness, offering additional clinical insight in certain cases.
Regular monitoring of intraocular pressure is essential because eye pressure can fluctuate over time. Tracking these changes allows ophthalmologists to identify trends and assess the risk of developing glaucoma. Early detection enables timely intervention, which can help preserve long-term vision. Consistent follow-up examinations play a crucial role in maintaining overall eye health.
The Difference Between Ocular Hypertension and Glaucoma
Ocular hypertension and glaucoma are often confused, but they are not the same condition. Both involve pressure inside the eye, yet the impact on eye health is very different. Understanding the difference can help people feel more informed and less worried about their diagnosis. It also highlights why regular eye examinations are so important.
Ocular hypertension means the pressure inside the eye is higher than normal, but there is no damage to the optic nerve and no loss of vision. In most cases, it does not cause noticeable symptoms, and vision remains clear. It is not considered an eye disease on its own, but it does need monitoring. Doctors usually keep a close watch to ensure it does not progress.
Glaucoma, however, is an eye disease that damages the optic nerve and can lead to gradual vision loss over time. It is often linked to raised eye pressure, although this is not always the case. You can think of ocular hypertension as a warning sign rather than a disease itself. While it increases the risk of developing glaucoma, not everyone with ocular hypertension will go on to develop the condition.
Risk Factors for Progression to Glaucoma
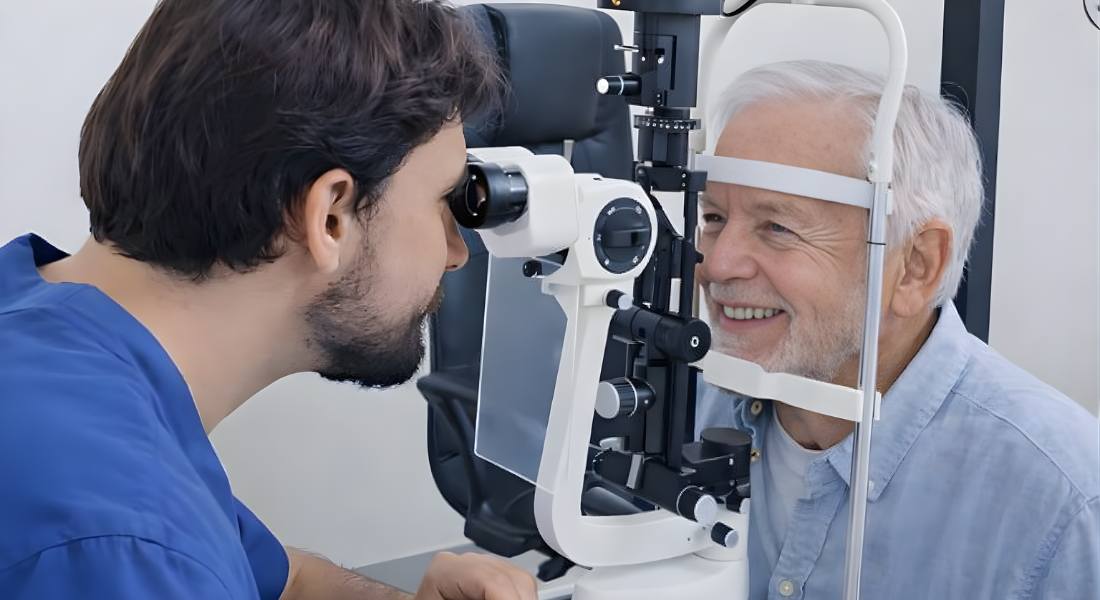
Understanding your individual risk is essential when monitoring ocular hypertension. Not everyone with raised eye pressure will develop glaucoma, but certain factors can increase the likelihood of progression. Identifying these risks early allows for better planning and closer observation. Your eye specialist will carefully assess your overall situation before making any decisions.
One important factor is the level of eye pressure, as higher pressure generally increases the risk of optic nerve damage. Age also plays a role, with older adults being more likely to develop glaucoma over time. A family history of glaucoma can further raise your risk, as genetics may influence how your eyes respond to pressure. In addition, thinner corneas can affect pressure readings and may be linked to a higher chance of progression.
Other eye conditions, such as myopia (short-sightedness) or structural changes in the optic nerve, may also increase susceptibility. These factors do not guarantee that glaucoma will develop, but they are important considerations. Your ophthalmologist will take all of these elements into account when deciding whether simple observation or active treatment is most appropriate. Regular monitoring ensures that any changes can be detected at an early stage.
Symptoms and Signs
Ocular hypertension usually does not cause any noticeable symptoms. Most people are unaware they have raised eye pressure until it is detected during a routine eye examination. Vision generally remains clear, and there is no pain or obvious discomfort. This is why many cases are discovered by chance during regular check-ups.
Because it develops silently, ocular hypertension can easily go unnoticed for years. People often feel completely normal and may not suspect any issue with their eyes. Regular eye tests are therefore essential, even if your vision seems perfectly fine. Early detection allows your optometrist to monitor the condition closely.
Glaucoma, by contrast, often progresses slowly and quietly as well. Vision loss can occur gradually and may not become noticeable until the condition is more advanced. By the time symptoms appear, some damage may already be permanent. Detecting raised pressure early is one of the most effective ways to help prevent long-term harm to your sight.
Diagnostic Assessments
Monitoring ocular hypertension and detecting the early stages of glaucoma require a comprehensive and systematic approach. Ophthalmologists rely on a combination of specialized diagnostic tests to evaluate both eye pressure and the health of the optic nerve. Since glaucoma can progress silently without noticeable symptoms, these assessments play a critical role in early detection. Regular testing ensures that even subtle structural or functional changes are identified promptly.
- Visual Field Testing: Visual field testing evaluates peripheral (side) vision to detect subtle vision loss that may not be noticeable to the patient. Early glaucoma often affects peripheral vision first, making this test especially valuable for early diagnosis. Identifying small defects allows for earlier intervention before central vision becomes compromised.
- Optical Coherence Tomography (OCT): Optical Coherence Tomography provides highly detailed cross-sectional images of the optic nerve and retinal nerve fibre layer. It helps detect thinning or structural damage that may occur before vision loss is measurable. This imaging technology allows ophthalmologists to monitor progression with great precision over time.
- Tonometry: Tonometry involves repeated measurements of intraocular pressure to identify fluctuations or sustained elevation. Since eye pressure can vary throughout the day, consistent tracking helps establish trends. These measurements guide decisions regarding treatment initiation or adjustment.
- Gonioscopy: Gonioscopy is used to examine the drainage angle of the eye, where fluid exits to regulate pressure. This test helps determine whether the angle is open or closed and rules out secondary causes of increased pressure. Understanding the drainage system’s condition is essential for accurate diagnosis and management planning.
When performed regularly, these diagnostic assessments provide a comprehensive picture of eye health. They allow ophthalmologists to detect early damage, evaluate risk, and tailor treatment strategies accordingly. Early and consistent monitoring significantly reduces the risk of vision loss. Through careful evaluation and follow-up, long-term visual health can be effectively preserved.
Lifestyle Factors and Eye Pressure
Although not all risk factors can be controlled, certain lifestyle choices may help support healthy eye pressure. Small, consistent changes can make a positive difference over time. These habits should not replace medical treatment, but they can work alongside it. Maintaining overall wellbeing often benefits your eyes as well.
Regular exercise, particularly moderate aerobic activity such as walking or cycling, may help to lower eye pressure slightly. A balanced diet that includes leafy green vegetables, omega-3 fatty acids, and antioxidants can support overall eye health. Avoiding smoking is also important, as smoking increases the risk of many eye diseases, including glaucoma. Making healthier choices each day can help protect your vision in the long term.
It is also wise to limit caffeine intake, as high amounts may temporarily raise eye pressure in some people. Paying attention to daily habits can help you feel more in control of your eye health. These lifestyle adjustments are simple but meaningful steps. When combined with regular eye examinations, they can contribute to maintaining healthy vision over time.
Treatment Options
Treatment for ocular hypertension is not always required, as some people can be safely monitored without immediate intervention. Your ophthalmologist will carefully consider your level of risk before recommending any treatment. The aim is to lower eye pressure if the benefits outweigh any possible side effects. Decisions are always based on your individual circumstances and overall eye health.
For many patients, observation and regular monitoring are sufficient, particularly if the risk of developing glaucoma is low. This usually involves eye pressure checks every six to twelve months, along with periodic OCT scans and visual field tests to assess the optic nerve. Lifestyle advice may also be provided to support long-term eye health. Close monitoring ensures that any early signs of change can be detected promptly.
If treatment is needed, eye drops are the most common option for lowering intraocular pressure. These include prostaglandin analogues, which improve fluid drainage, beta blockers and carbonic anhydrase inhibitors, which reduce fluid production, and newer rho kinase inhibitors that also help lower pressure. Laser procedures such as Selective Laser Trabeculoplasty and Argon Laser Trabeculoplasty can improve drainage and may reduce the need for daily medication.
Monitoring and Follow-Up
Regular follow-up appointments are essential when managing ocular hypertension. These visits help detect any early changes before permanent damage can occur. In most cases, reviews are scheduled every six to twelve months, although they may be more frequent if your risk factors are higher. Consistent monitoring provides reassurance and supports timely decision-making.
During these appointments, several tests are usually carried out to assess eye health. These may include tonometry to measure eye pressure, OCT scans to examine the optic nerve, visual field assessments, and a full eye examination. Each test provides important information about whether the condition remains stable. Together, they help your ophthalmologist track even small changes over time.
Patient awareness also plays an important role in ongoing care. Keeping note of any changes in vision, new eye discomfort, or updates to your family medical history can be helpful. Sharing this information during appointments ensures a more complete assessment. Active monitoring allows early intervention if needed, giving you the best chance of preserving your vision.
Misconceptions About Ocular Hypertension
Being diagnosed with ocular hypertension can cause unnecessary worry for many people. It is common to assume the worst, especially when eye pressure is mentioned. However, several misunderstandings surround this condition. Learning the facts can help you feel calmer and more confident about your care.
One common misconception is the belief, “I will definitely get glaucoma.” In reality, only a proportion of patients with ocular hypertension go on to develop glaucoma, and many never experience further problems. Another concern is, “I need surgery immediately,” but most people are managed safely with regular monitoring or prescribed eye drops. Treatment decisions are always based on individual risk rather than fear.
Some patients also worry that long-term use of eye drops is harmful. Modern medications are generally safe and are carefully prescribed to minimise side effects. Your ophthalmologist will monitor you to ensure the treatment remains suitable and effective. Understanding these points allows you to take a balanced and informed approach to protecting your vision.
When to Seek a Specialist

Ocular hypertension requires careful monitoring to prevent potential damage to the optic nerve. While regular eye exams are essential, certain situations call for evaluation by a glaucoma specialist. Early expert intervention can help reduce the risk of developing glaucoma and preserve long-term vision. Seeking timely care ensures that any changes in eye pressure are properly assessed and managed.
- Consistently High Pressure Readings: If intraocular pressure remains elevated over multiple visits, specialist assessment becomes important. Persistent high readings may increase the risk of optic nerve damage. A glaucoma expert can perform advanced testing to determine whether treatment is necessary.
- Presence of Additional Risk Factors: Individuals with a family history of glaucoma or thin corneas face a higher risk of progression. These factors can make the optic nerve more vulnerable to damage. A specialist can evaluate overall risk and recommend a tailored monitoring or treatment plan.
- Early Warning Symptoms: Symptoms such as blurred vision or loss of peripheral vision may indicate early glaucoma. Although glaucoma often develops silently, any noticeable visual changes should not be ignored. Prompt specialist evaluation can help detect problems at an early stage.
Clinics offering advanced care, such as those providing glaucoma treatment in London, use detailed diagnostic imaging and personalised care plans to manage eye pressure effectively. Early referral to a specialist improves the chances of preventing disease progression. Proactive management can protect vision and provide reassurance. Regular follow-up combined with expert guidance offers the best strategy for maintaining eye health.
Supporting Eye Health at Home
Supporting your eye health at home is an important part of long-term care. While medical treatment plays a key role, daily habits can also make a meaningful difference. Simple and consistent actions help protect your vision over time. Taking responsibility for your eye health can give you greater confidence and control.
Maintaining regular check-ups and attending all recommended tests ensures that any changes are detected early. It is equally important to use prescribed medications exactly as directed, as consistency is essential for them to be effective. Protecting your eyes from injury and excessive UV exposure, such as by wearing suitable eyewear, can also reduce unnecessary risk. These steps work alongside professional care to maintain stability.
Managing general health conditions, including blood pressure and diabetes, is another vital aspect of eye health. Good overall health supports healthy blood flow to the optic nerve and surrounding structures. By taking a proactive and informed approach, you reduce the likelihood of future complications. Small, steady efforts can have a lasting impact on preserving your vision.
The Role of Early Detection
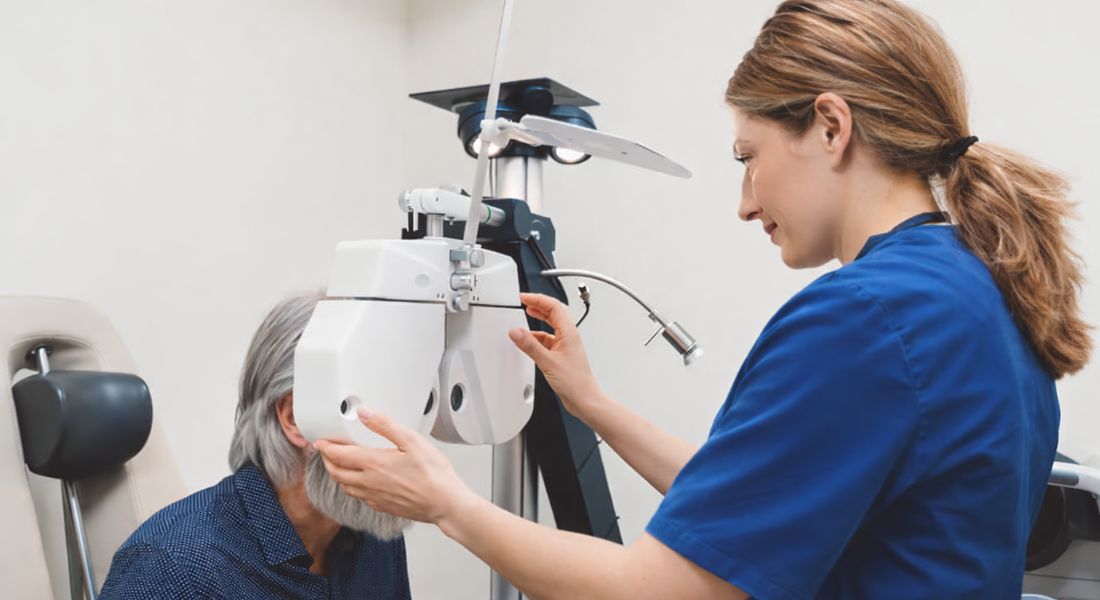
Early detection plays a vital role in preventing vision loss from glaucoma. Ocular hypertension can act as an important warning window, giving doctors time to assess potential risk. When raised eye pressure is identified at an early stage, action can be taken before damage occurs. This proactive approach greatly improves long-term outcomes.
By detecting elevated eye pressure early, your ophthalmologist can carefully assess and stratify your risk of progression. They can then decide whether simple monitoring or active treatment is the most appropriate course of action. Regular reviews allow small changes to be identified before they become serious. This helps to protect the optic nerve and maintain stable vision.
Routine eye examinations are therefore essential, especially if you have a family history of glaucoma or other risk factors. Even when vision seems normal, important changes can be developing without obvious symptoms. Early diagnosis provides the best opportunity to preserve sight for the long term. Consistent check-ups remain one of the most effective safeguards for your eye health.
Summary of Key Points
Ocular hypertension refers to raised eye pressure without any damage to the optic nerve or loss of vision. It is not the same as glaucoma, although it can increase the likelihood of developing it over time. Importantly, not everyone with ocular hypertension will go on to develop glaucoma. Careful assessment helps determine individual risk.
Several factors influence the chance of progression, including age, family history, corneal thickness, and the level of intraocular pressure. These elements are considered together rather than in isolation. Management may involve regular monitoring, healthy lifestyle adjustments, prescribed medications, and in some cases laser therapy. The approach chosen depends on your specific level of risk.
Early detection remains the most important factor in protecting long-term vision. Routine eye examinations allow raised pressure to be identified before permanent damage occurs. Ongoing follow-up ensures that any changes are addressed promptly. With the right care and monitoring, many people maintain stable and healthy vision.
FAQs:
- What is ocular hypertension?
Ocular hypertension is a condition where the pressure inside the eye (intraocular pressure) is higher than normal, but there is no damage to the optic nerve and no vision loss. - Does ocular hypertension always lead to glaucoma?
No, ocular hypertension does not always lead to glaucoma. While it increases the risk, many people with raised eye pressure never develop optic nerve damage. - What is the difference between ocular hypertension and glaucoma?
Ocular hypertension involves elevated eye pressure without nerve damage. Glaucoma is an eye disease that causes optic nerve damage and can lead to vision loss. - What is considered a normal eye pressure range?
Normal intraocular pressure typically ranges between 10 and 21 mmHg. Readings consistently above this range may indicate ocular hypertension. - Are there any symptoms of ocular hypertension?
Ocular hypertension usually does not cause noticeable symptoms. Most people discover it during a routine eye examination. - How often should eye pressure be checked?
If you have ocular hypertension, your ophthalmologist may recommend monitoring every 6 to 12 months, depending on your individual risk factors. - What are the risk factors for developing glaucoma from ocular hypertension?
Risk factors include higher eye pressure levels, increasing age, family history of glaucoma, thin corneas, and certain structural changes in the optic nerve. - Can lifestyle changes help lower eye pressure?
Yes, moderate exercise, a healthy diet rich in leafy greens, limiting caffeine intake, and avoiding smoking may support healthy eye pressure, though they do not replace medical treatment. - When is treatment necessary for ocular hypertension?
Treatment may be recommended if your risk of developing glaucoma is high. This may include prescription eye drops or laser procedures to reduce intraocular pressure. - Can vision loss from glaucoma be reversed?
No, vision loss caused by glaucoma is permanent. However, early detection and proper treatment can prevent or significantly slow further damage.
Final Thoughts: Staying Informed and Protecting Your Vision
Being diagnosed with ocular hypertension can feel unsettling at first, but it is important to remember that it is a risk factor, not a disease. Raised eye pressure does not automatically mean you will develop glaucoma. With regular monitoring, personalised risk assessment, and timely intervention when needed, most people maintain stable vision and avoid long-term complications.
The key is consistency. Attending scheduled eye examinations, following professional advice, and addressing any changes early provides the strongest protection for your eyesight. Modern diagnostic tools and treatment options have made it possible to detect problems earlier than ever before and manage them effectively. If you’re exploring whether glaucoma treatment in London could benefit you, get in touch with us at Eye Clinic London to schedule your consultation. Proactive care today can make all the difference in preserving your vision for the future.
References:
- Nandzik, M., Wylęgała, A., Szkodny, D., Wróblewska-Czajka, E., Wylęgała, E. and Orzechowska-Wylęgała, B., 2024. Risk Factors for Glaucoma and Ocular Hypertension and Post-Transplant Complications in Keratoconus: A Multivariable Analysis. Journal of Clinical Medicine, https://www.mdpi.com/2077-0383/13/18/5407
- Liu, T., Cai, Y., Hu, M., Wang, Z., Liu, X., Chen, M. and Wang, K., 2025. The Impact of Intraocular Pressure Fluctuations on the Progression of Glaucoma and Associated Factors. Advances in Ophthalmology Practice & Research https://pubmed.ncbi.nlm.nih.gov/40276029/
- Medeiros, F.A., Weinreb, R.N., and Rao, H.L., 2023. The Natural History of Untreated Ocular Hypertension and Glaucoma: Structural and Functional Progression. Survey of Ophthalmology https://www.sciencedirect.com/science/article/abs/pii/S0039625722001746
- Qureshi, I.A. and Xi, X.R., 1997. Intraocular Pressure, Ocular Hypertension, and Glaucoma: A Comparison of White and Blue Collar Workers. Journal of Occupational Health https://academic.oup.com/joh/article/39/3/211/7270525
- Decision Factors for Glaucoma Suspects and Ocular Hypertensive Treatment at an Academic Center, PMC, 2019. Ocular Hypertension Treatment Study (OHTS) data on conversion rates to glaucoma https://pmc.ncbi.nlm.nih.gov/articles/PMC10618603/

